Do you need to know the precise reason why your knee hurts?
Knee and shoulder pain is widespread. Most people in my office do not recall a specific injury. They’re confused and do not know why something hurts. They’ve read about meniscus tears and rotator cuff tears… they’re scared, and everything they read online says that they need surgery. Of course, they will want to be referred for an MRI.
Most people want to know specifically what is wrong with them. They want a name, a structure… more esoteric discussions about how joints can hurt sometimes and if we wait long enough, it usually feels better often fall on deaf ears.
There are costs associated with that desire to know specifics. First, many studies have shown that a good doctor who listens to you and examines you can often tell you what is hurting you with reasonable precision. Your story, your description, and our examination are often more successful than an MRI at determining what hurts. The investigation can often stop there… but it usually doesn’t. The cost of that visit… perhaps $75 for a visit and $100 for an X-ray. But medicine has become a high-tech low-touch science. Most patients are cut off from speaking in 18 seconds. A cursory examination at best is performed. Then a brace is given ($300-$1000), an injection might be given ($150-300), an MRI will be ordered ($300-$4000)… and then the physical, emotional costs of viewing your MRI results, overdiagnosis, and over-treatment might kick in. What’s the cost of you never wanting to run or work out again?
An MRI shows structures— ligaments, bones, cartilage, tendon, and muscle. An MRI cannot show us what hurts. Moreover, most people, some doctors included, do not understand what the normal “age-appropriate” changes on an MRI should be. This is the perfect setup for the possibility of increasing the risk calculus of your interaction in the doctors’ office.
Stephanie was an endurance trail runner. She kicked my butt on almost every local trail run. She climbed hills like a mountain goat, and only her toes briefly touched the ground during each stride.
Do you know why my joint hurts?
I guess it’s only natural to want to know precisely what’s “wrong” and what’s hurting. I imagine that the same might have been true for me in my earlier decades. That desire for a specific name, or diagnosis, could initiate a spiral. One that might work out well in the end… or it might be the end of your running or cycling career. And the odds on which path you might find yourself on are not favorable.
Face it… changes occur due to aging. We don’t think twice about the need for glasses, graying hair, balding and other issues we look past every day. Why do we expect the inside of our joints to be as neat and perfect as they were when we were 16 years old?
Healthcare is a business… one that is fed by diagnoses
An important issue to understand: Medicine is a business. The healthcare industry drives a large percentage of our GDP. And a large percentage of that spend is unnecessary. But wait… something hurts me; certainly more tests are better, no? No! I’ll elaborate later…
The potential drivers for overdiagnosis
- Lack of time. Medicine is a business! Volume is critical. Doctors are assessed by their “productivity” or RVUs. It’s easier to order a test, than to explain why that test isn’t needed. These silly Press-Ganey scores that we receive drive how happy the hospital is with us. Well… if you didn’t give someone a narcotic they insisted on, or order a test they wanted, but wasn’t necessary— guess how that person will grade our “performance” on that day? It’s easier to order the test and please you.
- Insufficient training. Most training programs do not expose their residents to enough office time. Therefore residents see us operating on meniscus or rotator cuff tears all the time. They did not see the 100 patients from the prior few weeks that didn’t need surgery. Accredidation reqirements for residency are mostly focused on surgical volumes— not necessarily how the decision to operate was arrived at.
- Financial incentives. MRIs and other tests increase revenue streams, so do unnecessary braces, surgeries, orthotics, etc. This is why surgeons are paid more than non-procedural doctors. In the perfect world, your primary care doctor would make more than any surgeon. And paid well only if their patients are healthier. That’s not how things currently work.
- Uncoordinated care.
- Vested interests.

Stephanie twisted her knee during one of our runs. Rocks under leaves are a bit treacherous. She continued running that day, but her knee was swollen the next morning. She was worried and went for an X-ray at a local Urgent Care center, and that was normal. She went online and scheduled a visit to see an Orthopedic Surgeon the next day.
Many MRI “abnormalities” are, well… normal.
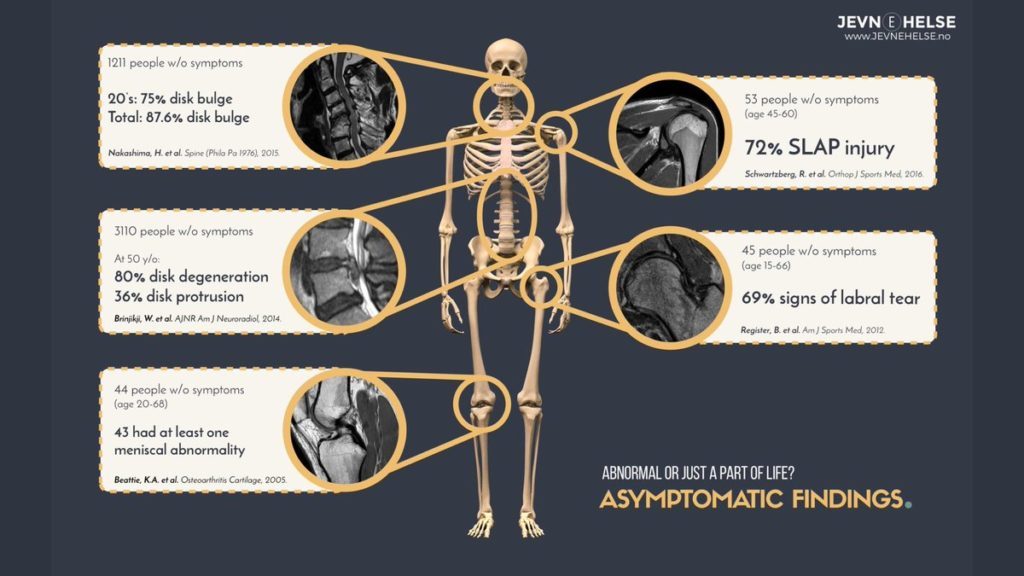
“Age-appropriate” findings on MRI readings are vastly under-appreciated. If you are over 50, have no pain, and place you into an MRI, you have at least a …
- A 20% chance of having a meniscus abnormality.
- An 80% chance of something being listed as an abnormality in your knee.
- A 10-15% or higher chance of having a rotator cuff tear.
- An 80% chance of having a disc bulge in your back or neck.
- This post explored MRI changes seen in the shoulders of people with no shoulder pain.
You cannot unsee your MRI result. I have witnessed many people who have shut down activities because something was seen on their MRI, and they cannot believe that exercise will not make it worse.
Humans die of very predictable causes, and your risk of dying from one of them is decreased significantly by moving and exercising. You’re not going to stop these age-appropriate findings from progressing… so don’t increase your risk of dying prematurely because you think you’re saving your knee, back, or shoulder.
We can run with meniscus tears… many of us do and don’t even know we have one. We can run if we have osteoarthritis, and running does not cause osteoarthritis, and running does not cause your osteoarthritis to worsen.
Imagine this; you’re a runner, you’re 52… there’s a 20% chance that you have a meniscus tear. Remember, these tears are very often not a cause of pain. One day your knee hurts… well— because these things happen. You go for an MRI. The meniscus tear is seen… but we can’t date these tears; we do not know when it occurred. Now you are exposed to the rising overtreatment wave in the US healthcare system. You might stop running because you think you’re injuring yourself. You might be told to stop running. Heck, you might be told you “need” an operation. All because you had an age-appropriate finding and some knee pain. How many 50+-year-old runners never have knee pain? Very few. This scenario is repeated thousands of times each day across our country. Many athletes will suffer financially, emotionally, and physically because of it.
A surgeon saw Stephanie. An MRI was obtained, and… it found a meniscus tear. Meniscus tears, especially posterior horn meniscus tears, are prevalent in runners. Indeed, that’s the cause of her pain? Right?!? Not necessarily. She was over 50, so there’s a good chance that the tear was there before the injury. She’s a runner; certainly, she needs an operation? Nope. Many “abnormalities” appear on an MRI of a runner’s knee. Most don’t require any formal treatment. There was a region of inflammation seen in the bone on her MRI. These are common findings in runners too. They resolve and are usually not an issue to worry much about. But surgery for a meniscus tear will not fix that boney inflammation…, and it stands a good chance of ruining her running career. Nonetheless… surgery was recommended.
Virtually nothing gets better in 6 weeks.
One thing is evident from personal experience and 20+ years of professional experience. We dramatically underestimate the time it will take for discomfort, swelling, etc., to resolve. Many overuse injuries such as rotator cuff-related pain, achilles tendon issues, tennis elbow, hamstring issues can take up to a year or more to resolve. Although this is off-topic for this post… avoiding overuse injuries by training properly is in your best interest.
The same goes for episodes of knee swelling. “Come back in two weeks, and if it’s not better, we can do the surgery.” Well… you might as well sign up for that surgery. It’s not going to resolve in two weeks. The swelling and discomfort might last for a few months. Athletes of all ages are prone to making emotionally laden poor decisions. Somehow we think that surgery will “fix” the problem and get us back out doing what we love sooner. That is true for some issues… but it is not valid for many other problems. Doctors have a role in this too. Medicine is a business. Second and even third opinions should be commonplace.

Stephanie had the surgery. The next time we ran together was one year later… and her knee is still swollen. Sometimes our joints want to recover at their own pace… and they don’t like being invaded and having pieces removed.








I salute for this honest writeup..it really upholds the way i have been practicing for last 30 years and often challanged for exactly the same views expressed by you..thanks a lot ..i felt vindicated today
Thank you so much for this post. I am a 79 year old female who has all of the age-appropriate aches and pains that you speak of. I feel so much better now about my bulging discs and achy knees after a couple of hours of tennis. My solution is to play every other day instead of every day. The off days are easy swim days or slow hiking/walking. I so appreciate your voice of reason. I plan to be reading your posts when I’m 99 and still playing, swimming, hiking.
That was very kind of you to share that. I’m super happy that you found this post useful.
Howard Luks
What about those aches and pains weightlifters (even moderate)have that can be fine for a while and then come back even though you are doing the same routine.
I have a recurring shoulder pain that I think comes from going too low – I have my worst case currently from {I think} doing press ups as a substitute for the weight bench during lockdown. Presumably it comes from going too low as I don’t do that with weights.
It no longer requires me to turn over in the night in a certain way to avoid the pain so maybe it is just time as per your point about pain taking a year to go away. from memory that is how it has been before – 6mth to 1year and 2 week breaks from the gym don’t do anything.
Philip.. This post was geared towards many broad scenarios… it certainly wasn’t meant to be inclusive of all injuries or aches. It was really in reference to those of us who just wake up one day with pain we didn’t have the prior day. We tend to overreact and push too fast for specific answers… when in fact just waiting is often the best answer. In your case, it might be different, it might not. At some point, it is worth getting a good physical examination, perhaps an Xray, ultrasound, MR, etc. Weightlifters, like runners, often bring these injuries on themselves. These aches/pains can often be training errors. Load management is critical. There’s a fair amount of research showing you do not need to workout with more than 65% of your 1rep max to gain strength or muscle mass. yes many continue to work out near their 1rep max. There also comes a point where it is time to get something checked out by a doctor… Good luck to you.
Howard, thanks for reply.
‘These aches/pains can often be training errors. Load management is critical.’
That’s probably it right there. I am using much less than 65% of my capabilities – ironically with the intention of minimising the risk of injury.
Hello from Canada!
Thank you for your website and the wonderful resources it contains. It is helping me make sense of a recent fall and injury to my left shoulder. I’m hoping if I provide a few details, you may be able to answer a few questions I haven’t been able to solve for:
– 55 year old female masters athlete – sustained acute traumatic injury to left shoulder while skiing 8 days ago
– visit to ER showed no fracture
– 8 days in, still unable to move arm out to side or front (not at all!) but can move it behind me and also use my forearm and hand as long as elbow is tucked into my side
– I have a referral for MRI and orthopaedic assessments
My questions:
1. If this injury is likely to need a surgical repair, how much time do I have before muscle/tendon retraction takes place?
2. How long before the dreaded “fatty muscle” sets in?
3. Is there anything I can do to slow this process?
3. I am a serious masters swimmer (average 10km per week) and dedicated kettlebell and body weight exerciser. I work as a dental hygienist. Assuming all goes well, how long before I can expect to return to these activities.
I would so appreciate your insight and knowledge as I attempt to manage my injury. Best regards from a wounded Canuck eh?
Lisa
Clearly, you have a reason to be imaged early.
Need to rule out a large rotator cuff tear.
You are not at risk for retraction or atrophy at this stage… unless their was a subclinical tear prior to this injury.
8-12 months for full return from these “massive” tears – IF that’s what it proves to be.
Good Luck