
Over-Testing and Over-Utilization of Healthcare Technology
I have utilized this blog on multiple occasions to discuss the issue of overuse and over-utilization of technology in healthcare. In a very broad sense this has tremendous implications not only with regards to the obvious cost involved— but over-utilization and overuse will foster further overuse and over-utilization because an *abnormal* finding will frequently lead to further testing and perhaps even unnecessary surgical intervention or invasive testing. I have discussed these issues, both here, here and here.
This very important article which came out of the New York Times yesterday, and was pointed out to me by my friend Wendy Swanson discusses the overutilization and overuse of MRI scans in the athletic population. This also clearly applies to each and every one of us. As I’ve mentioned in a previous blog post, our tissues change with age. There are many of you walking around out there with meniscus or cartilage tears in your knee— and simply don’t know it. There are many of you will walking around with tears in your rotator cuff, and simply don’t know it. Some of you may have herniated discs, evidence of osteoarthritis or other changes that clearly occur with age and activity – – – yet none of them are bothering you.
What Dr. Andrews found, was that when he obtained MRI scans on athletes with absolutely no discomfort or disability, the MRI found abnormalities in vital structures of the shoulder or knee in the vast majority of cases. Now, imagine that that athlete had shoulder pain after pitching one evening. Because they are a high-level athlete the typical process is that the athlete is placed into an MRI machine the very next morning and actions are undertaken based on the findings of that MRI. Now imagine the implications – – – Dr. Andrew’s study clearly shows that that athlete had close to a 90% chance of there being an abnormality before they even noted the onset of pain. Therefore, can we even be sure that the findings on the MRI are in fact meaningful, or more importantly, the source of discomfort. In many situations that athlete will be indicated for surgery because of the abnormal findings and find themselves on the sidelines and in the recovery process after having undergone a surgical procedure — which put them at significant risk — because of the risks and potential complications associated with surgery. In addition, especially in the high level athlete, very few high-level athletes return to their prior level of activity following certain procedures. Therefore, an over utilized or unnecessary at MRI could’ve potentially led to an unnecessary procedure which has now ended the career of the promising young young athlete.
Now is not a far reach to see how this affects you and the general population at large. You may have spent a long weekend outside cleaning the yard, playing soccer with the kids, or taking in a nice hike with your family. Or perhaps you simply twisted your knee and you have a little discomfort and difficulty walking the next day. For many of you. That will mean a visit to your physician’s office. For many of you. You may not be evaluated or examined and instead, to speed along the office-based visit. You’ll be given a prescription for an MRI. Now, in all likelihood, you also have or possess the same risk of having an abnormality on your MRI that would likely have been present prior to the onset of your discomfort. Please read that again! Now, you receive a telephone call from your primary care doctor that an abnormality was found on your MRI. You have a visit with an orthopedic specialist, hopefully that orthopedic specialists actually examines you, obtains your story, listens to your story, and determines whether or not the abnormalities identified could in fact be a competent producing cause of your symptoms. This does not always happen in the world of orthopedics today. Many practices focus on a high-volume, low touch – high-technology model where you will see a physician extender — the MRI abnormality will be identified, and quite possibly you will be indicated for surgery because of the finding. This nails home another concept I have discussed on here on many occasions. We treat patients, we do not treat MRI findings. We need to understand the personality of an injury and how that injury is presenting itself in you, how your lifestyle or quality of life is affected, and whether or not the findings that we have identified on the MRI are in fact the competent producing cause of your discomfort — and then come up with an appropriate treatment plan that will likely involve a period of nonsurgical management— which, if unsuccessful perhaps might lead to an indicated surgical procedure, if your lifestyle changes and quality-of-life dictates that this is in fact an option.
Do you have questions regarding an Orthopedic injury or longevity?
Do you want to talk to an expert who can listen to you for 45-60 minutes and explain the options in detail?
Dr. Howard Luks offers remote guidance sessions to review your X-ray or MRI images and explain your options.
Dr. Luks has also received hundreds of requests for educational sessions on the topics discussed in his book, Longevity Simplified.
Please do not approach your physician with the thought that an MRI is necessary in all situations where your knee, your elbow, or your shoulder bother you. Not all recent injuries require an MRI evaluation (some do). Please read this article carefully, the implications are significant—and we are talking about your body, your health, your pocketbook, preserving your quality-of-life, and protecting you from potentially harmful further testing and unnecessary surgery. And by all means…. use second opinions! That’s their primary purpose!








Eric
Hi Dr.Luks,
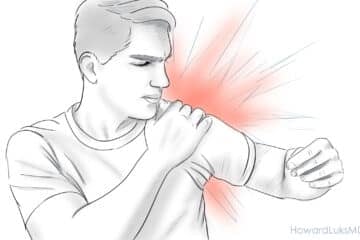
I was at the gym and had an acute injury accompanied by a loud pop when I pushed my shoulders back at a chest press machine with no weight. Prior to this my shoulder felt tight. My doctor found a small posterior labral tear in an MRI of my shoulder upon examination which corroborated the physical exam. My shoulder aches chronically and occasionally catches and pops. He claims this is the exclusive cause of my pain and that because it is small I would only need 1 week in a sling post surgery and 11 weeks of pt to get back to 100%. I suspect this means he is recommending debridement and wonder how it is possible to return to full strength post operation. I’ve tried some pt I learned from impingement in my other shoulder with only minor improvement. It has been about 5 weeks and am leaning towards surgery considering what he said. Is it possible to return to “full strength” after a debridement?
Thanks!
Eric
Stuart Hayward
Hi Howard, I am a 29 year old South African male marathon kayaker and middle distance swimmer. Over the past 2 years I have been guilty of overtraining- failing to do the necessary upper body strengthening exercises required to keep my body in top shape for upper body endurance exercise. Whenever I upped my kayaking training distance for marathons my left arm would get tensed up and eventually I would feel a “crunch” sound in my left shoulder. For months thereafter I would be sore and not do any overhead sport, until my arm felt better, when I would resume training, then it wuld happen all over agin- stupid I know…much regret. In December of 2012 I had my most recent crunch whilst kayaking, by June 2013 my arm sore from swimming, so I wnet for an PT and had an MRI- the MR confrmed a SLAP V- consistent with a Bankart Lesion and a SLAP lesion. I have since the beginning of November 2013 been suffering from horrible night pain in my left shoulder and a dull aching numbness in my arm during the day and pain whilst trying to change the gears in my car (referred pain throughout my left arm). The pain was so bad yesterday mornig that I went for a cortisone shot in my shoulder- this has relieved a great deal of pain. I have 2 opinions from 2 respected orthopaedic surgeons in Johannesburg, South Africa both gotten from my MRI and symptoms….1stly- one orthopaedic surgeon says that I most likely have glenohumeral arthritis caused by trauma to my glnohumeral cartilage in my left shoulder- no scope necessary now and 2ndly- the other orthopaedic surgeon says that a scope is necessary because something else other than arthritis could be causing my pain. What do you think? Is a scope a good idea? Even if a scope just serves to confirm glenohumeral arthritis and this would could allow pain relief from debridement and/or synovectomy- a scope would assist because then there would be no doubt and I could get some temporary relief. Unsure??? Please assist. I do not want to put myself through unncessary surgery… Perhaps I could e-mail you? my e-mail is [email protected] thanks in advance.
Stuart … When you put your complaints into context they are not consistent with your MRI findings. SLAP lesions and labral tears in general are not the typical cause of night pain. Either rotator cuff disease in the form of rotator cuff tendinosis, partial tears, etc are a very common cause of the symptoms you describe. Osteoarthritis, if it is severe can cause very similar symptoms too. The fact that you responded to an injection is very favorable.
Howard Luks
Carolyn
I injured my knees almost two months ago when I was at a stop light and hit by a driver going 80 mph. I’m currently stuck in PT limbo, with absolutely no imaging done on knees. No x-ray, no MRI. Just primary’s assumption that it is both knees meniscus (after insisting for 3 weeks that right leg was just overcompensating for left). Because of the much greater pain in one (left) that the other I am doubtful. I do not see ortho for another 2.5 weeks because they want to wait and see if I get better or worse with PT. My question is, at what point is it a serious concern that you are further injuring yourself by having no firm idea of the problem? I am not arguing with you but at this point I would give anything to know what the problem is. Walking hurts, sitting hurts, straight leg hurts. sleeping is impossible. Attitude is starting to suck.
There are times when an MRI becomes worthwhile. But they should not be used in isolation.. An MRI is typically performed to confirm a suspicion.
Stephen Rockower, MD
Treat Patients! Not MRIs!!! I hate when people demand MRIs “just to know what’s wrong” I ask if they are ready for the operation if it is “positive”. Of course not, they reply. So why do it? Sometimes its easier to just write the Rx and move on, though. Sigh
Thanks Stephen … Sadly this is the most widely utilized approach in healthcare today. Not only with regards to MRI… but for braces, medicines, etc…. Many physicians would rather write the script then spend a moment to explain why the test, brace or medicine isn’t necessary.
Unfortunately healthcare spending is unsustainable… and if we do not take more of an active role in controlling costs… someone is going to do it for us! :-( Big Sigh.
Martin Young
Excellent post! I have been saying for ages that doctors are encouraged, or rather forced in circumstances to practice high volume, low mark up, but by default low quality medicine, with all the consequences you have spelt out.
Hope that helps Bob!
Bob West
Think I Agree with your points, Howard. Unfortunately, I cannot distinguish your links from background due to color choices, so it’s difficulty to navigate the post properly. #colorblindness #sucks