
Cartilage regeneration has been a focus of Orthopedic Surgeons for decades. Cartilage damage or defects can occur after an injury such as an ACL tear. Cartilage has proven to be a very difficult tissue to work with… and it has frustrated researchers, surgeons, and patients. The FDA recently approved a process in the US known as MACI. Autologous chondrocyte implantation has been around for decades. The name implies that we biopsy and grow your own cartilage, then at a second procedure implant the grown cartilage back into your knee. Discussed in detail below, MACI offers surgeons a potentially more reliable method to regenerate cartilage damage in your knee.
Cartilage is a firm, rubbery substance that is on the end of your bones. Cartilage enables our joints to move and glide without any friction or any pain.
Cartilage can be damaged from auto accidents, falls, sports injury or as part of a degenerative or arthritic process. If the cartilage is damaged then there is a hole or defect in the surface that normally protects the bones of the knee. Those holes or areas of damaged cartilage can spread and lead to osteoarthritis.
Cartilage Regeneration:
Over the years the Orthopedic industry has tried many different techniques to fill these holes in the cartilage. One of the most commonly performed procedures is a microfracture. That is a procedure where we make many holes in the bone. Those holes allow bone marrow cells to enter the knee joint. Those cells will form a layer over the area of damaged cartilage. The issue with a microfracture is that it didn’t work for everyone and the new cartilage was not as firm or as strong as the cartilage you were born with. That issue led to other techniques to try and repair a cartilage injury. You can review those techniques here.
A technique known as an ACI was popular a while back. During an ACI we grew your own cartilage cells then placed them under a patch we sewed over the hole in your cartilage. That technique was met with mixed results — although when it worked the new cartilage was firmer and stronger. Vericel, the company that invented the MACI process appears to have improved upon the results obtained with the ACI procedure. In addition, they have simplified the procedure.
MACI procedure for cartilage regeneration

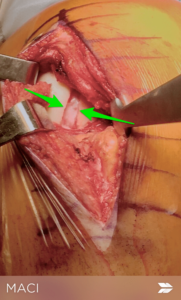
5-6 weeks is necessary to grow and implant the new cartilage cells onto the matrix. Then we bring you back to the operating room. This time we will make an incision in the front of your knee. The cartilage defect will be cleaned up and prepared. After proper preparation, we implant the new matrix with your cartilage cells into the defect. We attach the matrix to your knee with a biological glue or very small sutures.
Over the months after surgery, your cartilage cells will grow until the hole or defect in the damaged area of the knee is covered with new cartilage. The overall recovery is long and may require a period of time on crutches so you do not damage the new cells which they are growing. After a period of time on crutches, you will begin weight bearing exercises. The entire rehabilitation depends on the size of the defect or hole in the cartilage. The larger the hole, the longer the rehabilitation.
This paper shows that the MACI procedure appears to offer superior results when compared to a microfracture for cartilage regeneration. As with any relatively recent procedure, time will tell if the cartilage that grows is similar to the cartilage that you were born with. If the cartilage is of superior quality than MACI might offer Orthopedic Surgeons a new method to regenerate cartilage and minimize the risks of developing osteoarthritis.
Do you have questions regarding an Orthopedic injury or longevity?
Do you want to talk to an expert who can listen to you for 45-60 minutes and explain the options in detail?
Dr. Howard Luks offers remote guidance sessions to review your X-ray or MRI images and explain your options.
Dr. Luks has also received hundreds of requests for educational sessions on the topics discussed in his book, Longevity Simplified.
You can read more about the MACI procedure here.







Richard
Hi, I had cartilage removed in 1974. I have a little left, but not much. Would this treatment help mwith? If so how can I find a surgeon in my area that performs the procedure?
It is not a technology which is useful in a degenerative or arthritic knee. It is primarily used for cartilage defects due to trauma.
Stan
Dr. Luks,
Will this procedure work for patients with joint laxity or EDS – hypermobile type?
I don’t see why not. The key with proper patient selection for MACI is the type of cartilage defect. Traumatic cartilage defects are the best application of this technology. Trying to use this on degenerative or arthritic lesions is not likely to be met with success.
Brian
With a localized area due to trauma on the patella, what would you suggest if the microfracture fails? Thank you Dr.
Ben Portillo
Thanks Dr. This is good news/bad news. Good info/ bad that there is no solution. I have a 3 month old torn meniscus and mild narrowing in each knee. I now get cortisone shots in each knee every three months. Three months ago I had a GEL ONE (Hy acid)
I still get mild pain. Because of the meniscus tear, I have not played any tennis. I am 73 and normally play doubles 3-5 times a week. I wish to return to playing. That is why I was interested in the stem cell treatment. I see the Mayo is doing stem cell in their Rochester clinic only, but claims it is still is experimental. I shall research PRP here in Las Vegas. I shall order one of the braces that you have mentioned in blog. Also are there any supplements you recommend.
ben portillo
Hi Dr. I am interested in your option of stem cell for knee osteoarthritis. If good, which is better adipose, bone marrow, or both?
Is there material that i can read?
HI Ben …
There is NO evidence that stem cells will reverse arthritis and help you regrow cartilage. Unfortunately the internet is full of products with very empty promises and some at a very significant cost. Stem cells will likely work well in the future… but we are simply not there yet.
PRP injections or bone marrow injection (low WBC concentration) have been shown to help with the pain from arthritis. Some early research shows that PRP may also slow the progression of osteoarthritis.
Good luck
reflex8
Interesting article, any ideas about cartilage restoration at the back of the knee cap; it seems that Micro facture doesn’t help in this location.
You are correct… a microfracture is generally not successful on the patella. The type of treatment we recommend for patella cartilage defects depends on the type of defect. If the cartilage loss is spread out and due to arthritis it is treated differently then a localized area of injury due to trauma.
Brian
With a localized area due to trauma on the patella, what would you suggest if the microfracture fails? Thank you Dr.
Brian
Hello Dr, I had a MRI for right knee pain. It says I have a full-thickness defect of my articular cartilage in the middle of the trochlear groove, measuring roughly 10x6mm. Mild-moderate thinning of the articular cartilage over the central portion of the patella. My Dr wants to do a knee debridement and a microfracture if necessary. I am a very active person and have a physical type job. What approach would you recommend for the best long term solution for someone with an active lifestyle? Thanks in advance.
HI Brian …
The “best” procedure depends on a number of factors… sometimes we will try a microfracture for a small defect… but biopsy the cartilage for a MACI or ACI just in case the microfracture fails. That way you can avoid a second surgery to harvest the biopsy needed to grow your own cartilage. There is no consensus opinion on which is “the best” technique right now. Different techniques work best in different locations and with different size lesions. Most work better when there is no obvious evidence of degenerative or arthritic changes.
Brian
Thank you! Had a partial tear in the meniscus as well. He did microfracture the patella as it was small in size. 3 weeks removed, fingers crossed.