A high tibial osteotomy (HTO) is a procedure that we use to treat knee osteoarthritis swelling and pain, improve function, and often dramatically delay the need for knee replacement surgery. An HTO or osteotomy is a great option for those with knee joint osteoarthritis on mostly one side or compartment of the knee. An HTO is often recommended for people who want to return to a high level of activity like running or cycling. High tibial osteotomies are generally recommended for very active people such as athletes, hikers, runners, triathletes, and cyclists with knee arthritis swelling and pain that interferes with their ability to remain active.
Osteoarthritis and Malalignment of the knee:
Osteoarthritis affects different people in different ways. In some people, osteoarthritis may be limited to one side of the knee or one compartment. Arthritis can also be severe, it can be mild. Osteoarthritis can also affect the activities of people who suffer from it in very different ways. I know some people who can run with severely arthritic knees, yet others who can barely walk despite having mild arthritis on X-rays. The bottom line is, your experience with osteoarthritis will be unique to you. That’s why we need to cater a treatment plan that is also unique for you.
In order to understand how osteoarthritis might occur on only one side of the knee, we need to understand a little physics. If you have bowed knees, or what we call a varus knee, then the force going down your leg from the knee to the ankle is going through only the inner or medial side of your knee. Knees that are not bowed, or knock-kneed are in “neutral alignment” so that the force is going through the center of the knee joint. You place 4-7 times your body weight acr0ss the knee with every step. If one side of the knee is seeing the majority of that stress, the cartilage on that side will start to degenerate and become arthritic.
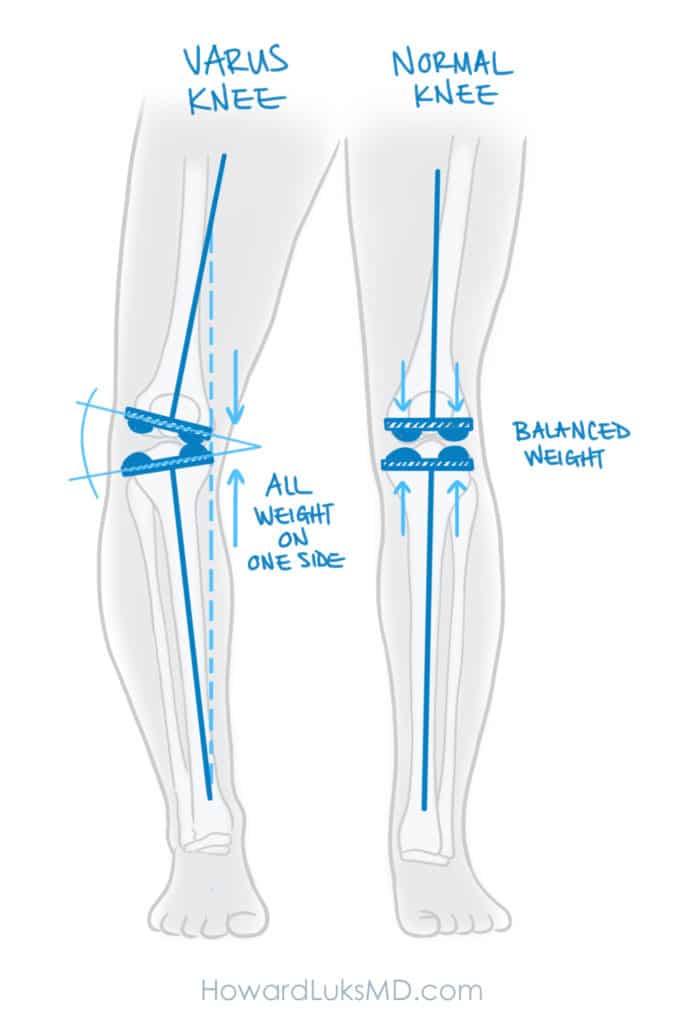
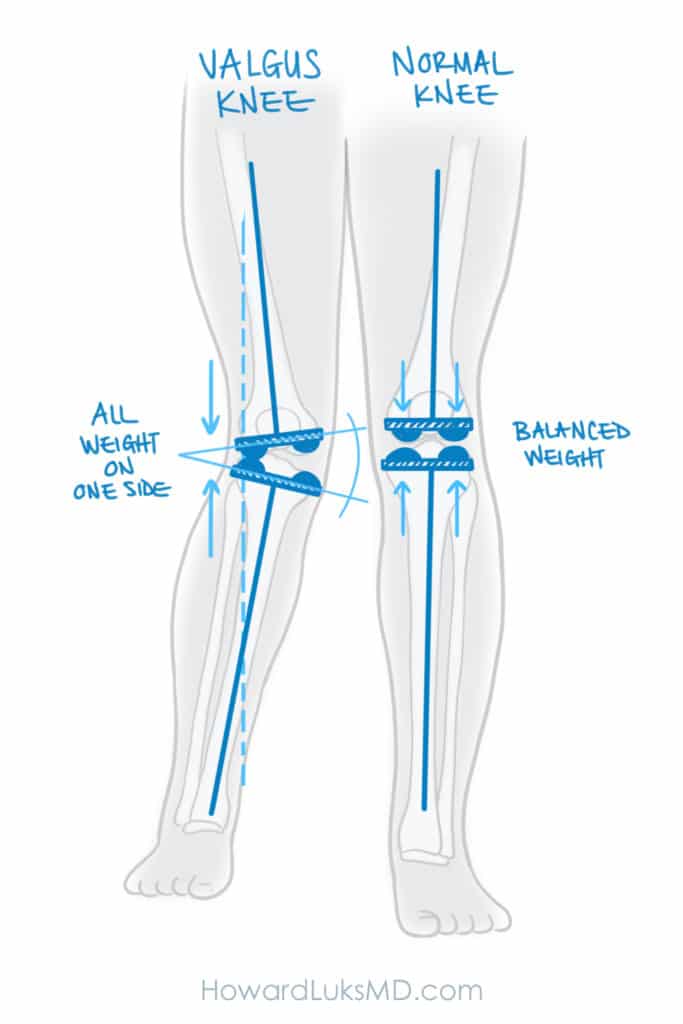
A similar issue can arise in people with knock knees or a valgus deformity. In this case, the force or weight is mostly going through the outside or lateral compartment of the knee.
Osteoarthritis that is limited to one side of the knee in a runner, cyclist, tennis player needs to be viewed differently than someone with osteoarthritis throughout the entire knee who can barely move around. Treatments are available to help alleviate the pain in both of these presentations… but those treatments might vary.
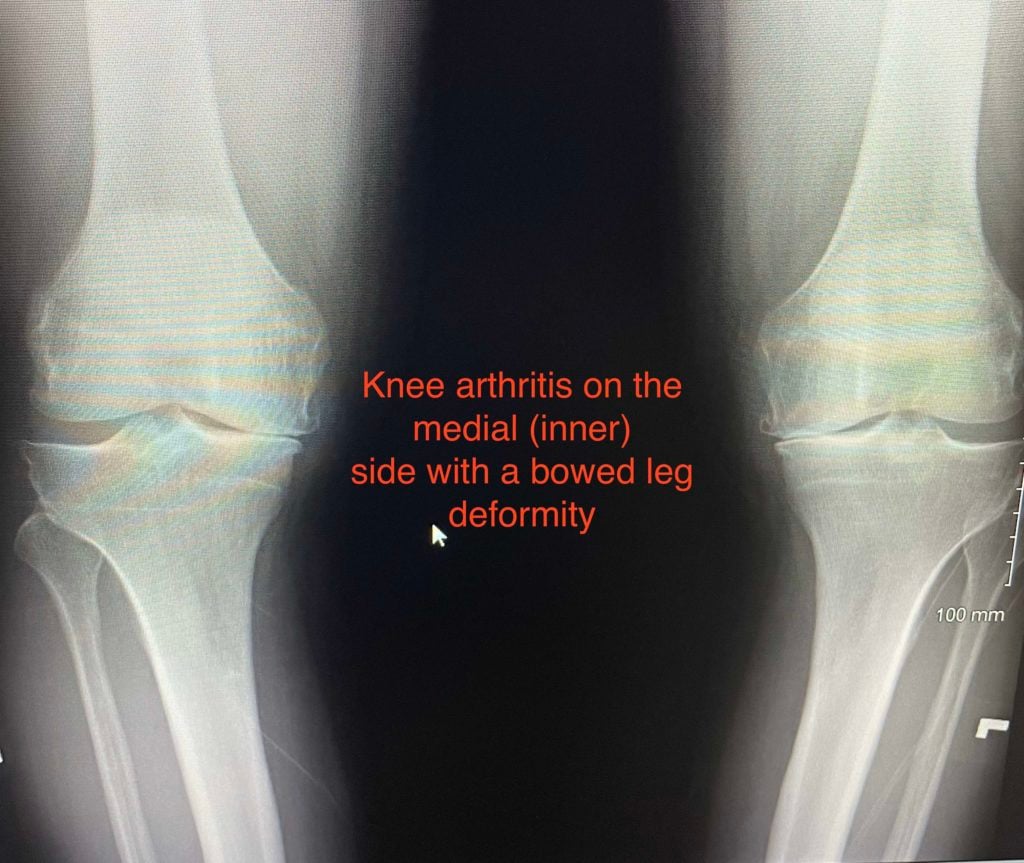
Here is a typical X-ray of an active person with a bowed leg and arthritis only on the medial or inner side of the knee. Notice how the space between the bones on the inner side of the knee is very narrow—this indicates thinning of the cartilage. The outer side of the knees maintains a normal space between the bones indicating that the cartilage thickness is normal. This is called varus arthritis, or varus arthrosis– simply put, deformity due to arthritis on only one side of the knee.
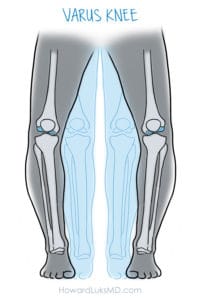
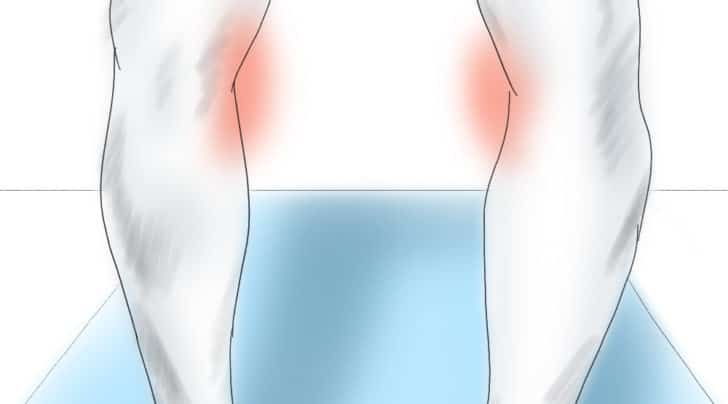
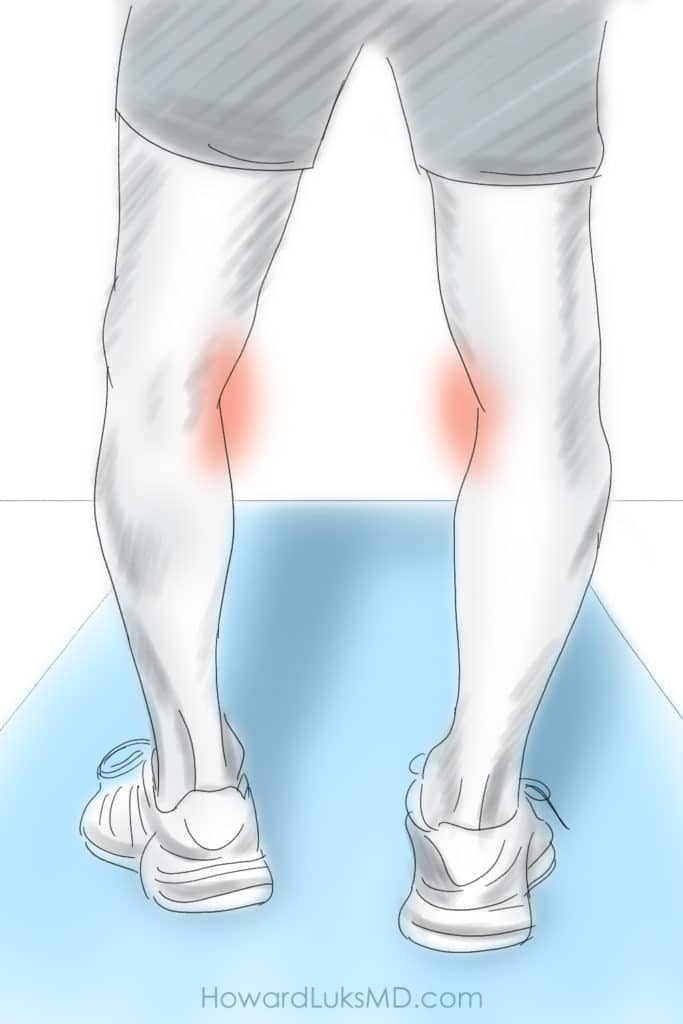
The typical person who will be a good candidate for a high tibial osteotomy is someone who is struggling due to medial or inner knee pain, during or after running, exercising, cycling, or playing tennis. Below is an illustration of how that X-ray above would present in the office. The legs are bowed outward, and the person would be complaining of pain mostly on the inner side. That pain can occur during an activity or after the activity.
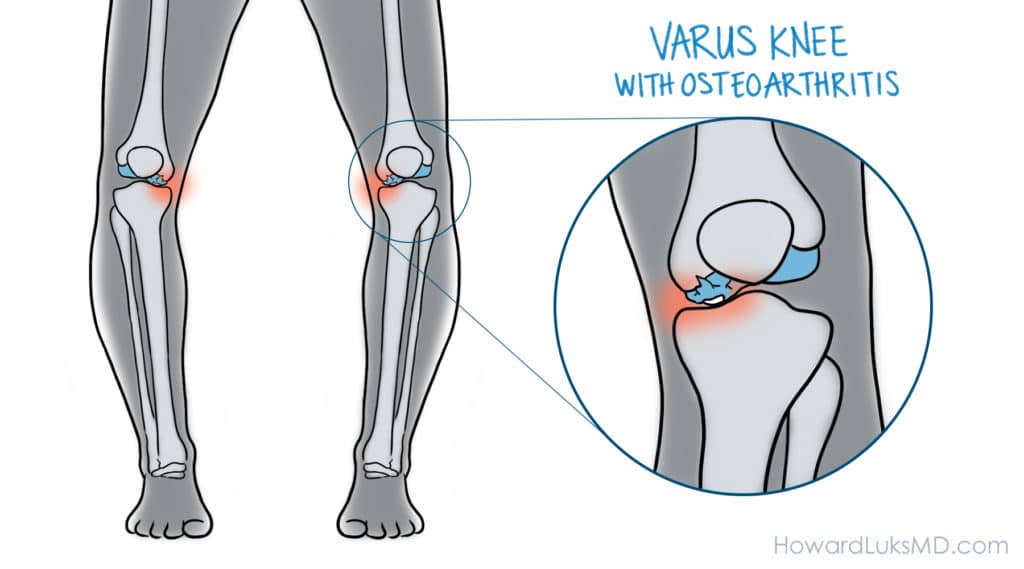
When you have a leg that is bowed, we call that a varus knee. When you have a leg that is knock-kneed, we call that a valgus knee. Both varus and valgus knees are a form of knee “malalignment”. Some people may have been born like this, but many of you developed knee joint malalignment after prior meniscus surgery or years after a knee injury.
What is osteotomy surgery?
In general, osteotomy surgery involves correcting the deformity in a leg so that the force or weight becomes more evenly distributed across both sides of the knee.
What is a High Tibial Osteotomy or HTO?
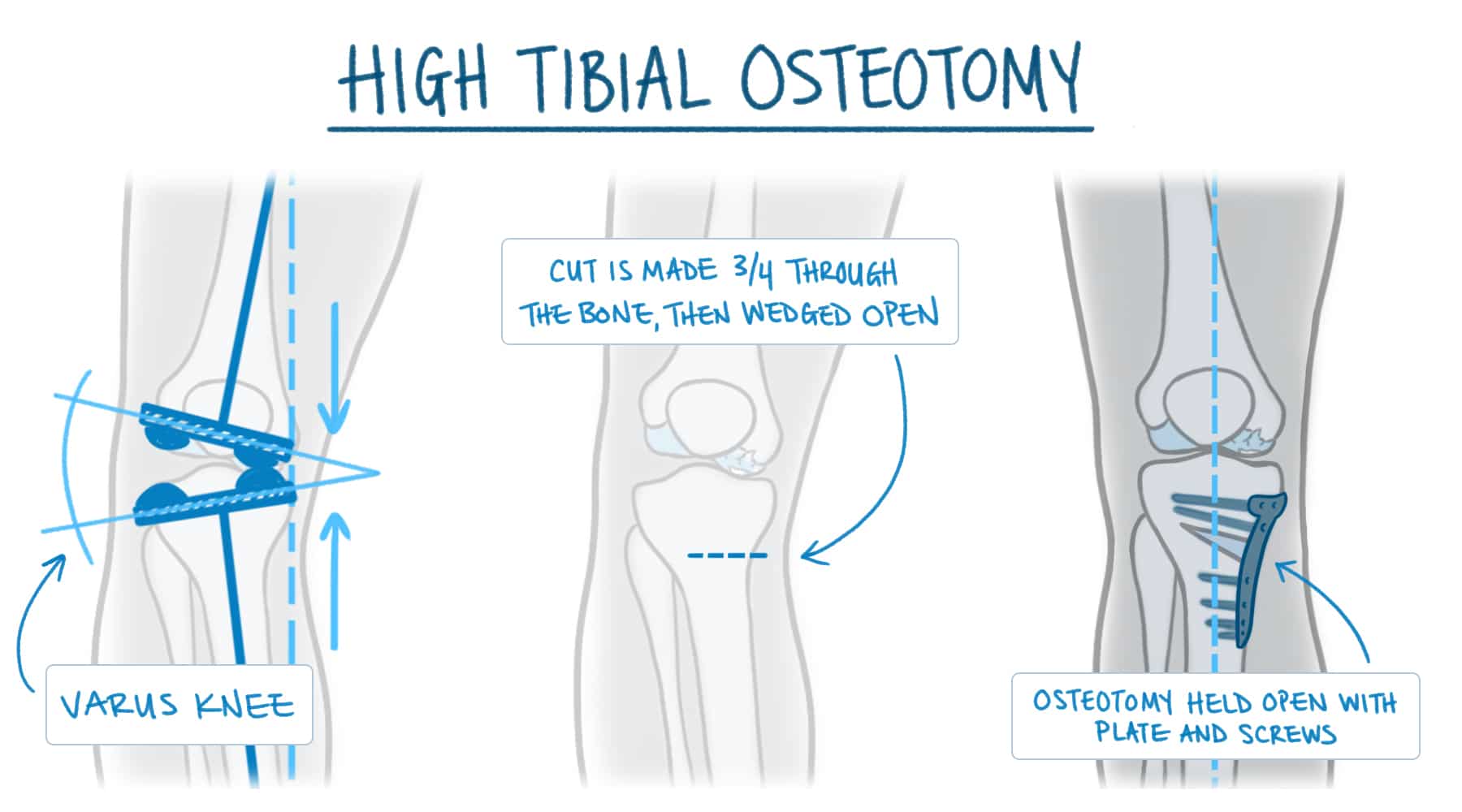
A high tibial osteotomy or HTO is a procedure we utilize to correct a varus or a bowed deformity of the knee. This is a form of knee malalignment. An HTO involves making a small cut through part of the tibia. We only cut one side of the bone, then we can open the cut to correct the alignment (see the image below). We need to open the cut in the tibia depending on how much of a correction we need to make to correctly align your leg.
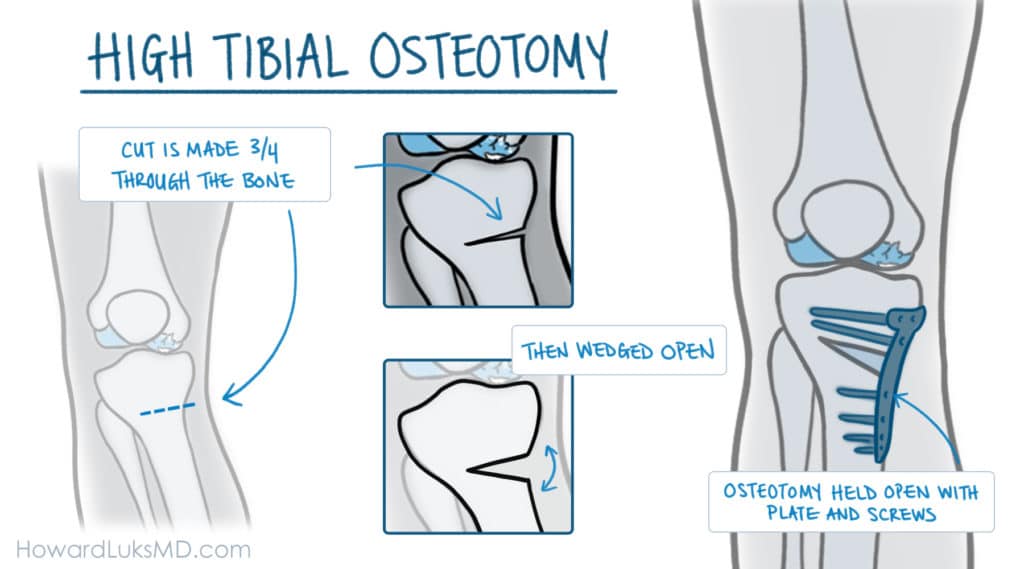
Ok.. take some deep breaths. Everyone gets a little concerned at this point when they realize we will be cutting their tibia. That’s a perfectly normal reaction… and honestly, that’s why I have created this post. Sometimes a much better understanding of the reasoning, rationale, and physics behind an HTO procedure can help a lot in your decision making.
It is important that you understand why we are recommending an HTO…
One more image… In the image below, the dashed blue line shows you where the line of force is during walking, or where all the stress is being felt by your knee. Every step you take transmits 4-5 times your body weight across the knee. That amount of stress adds up and leads to worsening arthritis over time. It will also increase the deformity over time. Notice on the picture on the left —that is a bowed or varus knee, the dashed line is coming through the medial or inner side of the knee. That is putting excess pressure on the cartilage and other structures in the medial compartment. That’s why most of you will also have a meniscus tear. The excess pressure in the medial compartment is causing the meniscus to degenerate too. Now, notice in the right image that the line of force or weight bearing is now coming through the center of the knee joint after the osteotomy. Thus, we have restored your alignment and now the side of your knee that had deteriorated and had become arthritic will no longer bear all the force of weight-bearing. This minimizes further degeneration and minimizes the pain that you had.
Which is better, an osteotomy or a knee replacement?
That’s a fantastic question. As I mentioned earlier, we need to look at the entire person. We are all different, some are sicker than others, some more active. Our goals matter significantly. I do not treat X-ray findings. I treat people. Each person is going to have a different story, a different set of complaints and issues, and a different set of goals. Their X-rays tell me only so much. Most runners, cyclists, athletes under 65 will do much better following an HTO than following a knee replacement. I am not knocking knee replacements… for the right person, they are a wonderful option too. If your arthritis is not isolated to one side of the knee and has spread throughout the knee then a knee replacement is often the better procedure.
I have been thankful to be part of a number of runners communities in my neck of the woods. Runners and athletes are often a little unique. We need to run to feel “whole”. It’s not so easy to just stop running. The majority of runners will not be able to run with a joint replacement. They certainly won’t run as well, nor as fast. When we utilize an HTO to restore alignment and minimize pain, we often enable very active people to return to their previously active lifestyles. We also avoid all the significant potential issues with knee replacements in very active people such as wearing them out, the need for another one in 10-20 years, the infection risk, and so on.
But I have a meniscus tear, isn’t that the cause of pain?
In many cases, the answer to that is no. In situations where you have pain on the inner side of the knee, and your knee is bowed or in varus, then you are overloading the inner or medial compartment of the knee. When we overload the medial compartment, we will see osteoarthritis, degenerative meniscus tears, and bone marrow edema- or inflammation in the bone itself. Failure to recognize that all of these are related to the varus alignment will result in an improperly indicated knee arthroscopy for a meniscus tear. Having an arthroscopy for a meniscus tear alone in a bowed or varus knee will often result in a knee that feels worse unless we c0rrect the malalignment and perform an HTO.

Who should consider osteotomy surgery?
Tibial osteotomy or an HTO should be considered in a young (<65 year old) healthy person who used to be very active, and athletic, and used to enjoy hiking, running, tennis, cycling, etc. When we evaluate you in the office, if we find that you have a bowed leg (it might be subtle), early arthritis in the knee, perhaps some swelling, and the arthritis is mostly limited to one side of the knee— then you will likely be a good candidate for an HTO.
Is a high tibial osteotomy painful?
Yes, an osteotomy is painful. But for most of you, it is not as painful as you expect. Most people are up and moving around very quickly. The bone is stabilized with a plate and screws so you will not feel the bones moving. Most of you will be able to start putting weight on your leg the same day as the surgery.
Do you have questions regarding an Orthopedic injury or longevity?
Do you want to talk to an expert who can listen to you for 45-60 minutes and explain the options in detail?
Dr. Howard Luks offers remote guidance sessions to review your X-ray or MRI images and explain your options.
Dr. Luks has also received hundreds of requests for educational sessions on the topics discussed in his book, Longevity Simplified.
Most HTO surgeries do not require an overnight stay in the hospital.
How long is the recovery from a high tibial osteotomy?
Your recovery will be unique to you. Most of you are allowed to put all your weight on the leg immediately after surgery. You will be on crutches for a few weeks. You will be encouraged to start bending the knee immediately. You will start physical therapy within the first week for range of motion and strengthening. Most of you will not require a brace. You will not require a cast.
Can I swim and cycle after osteotomy surgery?
Once the osteotomy has healed and your therapy has progressed to restore your strength and flexibility then you will be allowed to return to running, swimming, cycling, tennis, hiking, weight training, etc.
How successful is osteotomy surgery?
Osteotomy surgery is a successful procedure for the majority of people who have it. It helps alleviate or dramatically lessens the pain that you had prior to the procedure. In most studies, more than 60-70% of HTO patients have not undergone a knee replacement at 10-15 years after the HTO.
HTO surgery, utilizing contemporary planning and techniques does not complicate a future knee replacement.
Can you run after a high tibial osteotomy?
Yes. An HTO is offered with the understanding that you will be allowed to return to your prior activities. As with recovery from any injury or surgery, you will start off slowly and build back to your normal cadence, speed, and distance over time. Most runners who have a successful HTO are able to return to running. Does this mean that 100% of you will be able to run? No. The success rate of an HTO is very high… but we cannot guarantee all of you that you will be able to run.
How long is the scar or incision for an HTO?
Most patients are surprised that we can accomplish this procedure through a relatively small incision. Depending on the size of your leg, most HTOs can be accomplished through a 3-4 inch incision.
Can I drive after an HTO?
If you are having surgery on your right leg, then you will not be allowed to drive for nearly 6 weeks. If the surgery is on your left knee, then you can drive as soon as you can get into the car comfortably, and are off of narcotic pain medication.
Will I need physical therapy after an HTO?
Yes. You will need to work with a physical therapist. Initially, they will help you restore the range of motion to the knee. As the osteotomy starts to heal, they will progress your resistance exercises to help you gain back your strength. When your osteotomy is healed, they will help you safely return to your desired activities.
What are the risks of a high tibial osteotomy?
Any surgery involves risk. Many of the risks associated with an HTO are similar to those of any lower extremity surgery.
- Infection: The risk of infection is very low, but not zero. Most infections are treated with antibiotics. On occasion, we need to open the incision to clean it out.
- DVT or a blood clot in the leg. A small percentage of blood clots in the leg travel to the lung to cause a pulmonary embolus. Those can be dangerous.
- Failure to meet your goals.
- Risks of anesthesia. Very low in healthy people.
An HTO involves cutting through a portion of your bone. So that adds additional risks.
- Nonunion: this means that the bone doesn’t heal. The non-union rate of an HTO is very low.
- Hardware failure. That means that the screws we use to hold the osteotomy in position might break. This is a very rare complication. It happens if you try to do too much too soon, and it happens if the osteotomy doesn’t heal fast enough.
- In some people, especially those who are very thin, the plate and screws will be bothersome and have to come out. This involves a second procedure to remove the hardware after the bone is healed.
Because this procedure is being performed for osteoarthritis, there is a chance that you will continue to have pain. An HTO does not reverse the arthritic process, it dramatically slows down its progression because it takes the excess stress off the arthritic side. You will still have arthritis after the surgery, but you usually feel better because the inner side of the knee no longer is under very high stress or pressure.
Please read my disclaimer
Meet the illustrator… She’s wonderful!
Loraine Yow. https://www.lolo-ology.com