
Physicians who run tend to have many patients who run. Word gets around. Runners understand runners. And runners are often not an easy group to treat. That’s because they can’t stop running. A physician who is not a runner might not understand that. It’s too easy for many docs to say “You should stop running”.
Runners feel complete when they run. They run for exercise, they run to meet their daily aerobic threshold, but more often they run because it makes them happy and allows them to feel whole.
The effects of being an active runner go far beyond the aerobic fitness level one achieves. Personally, my days are often far easier to complete if I ran before getting to the office or if I know I get to hit the trails when I get home. Even my children notice the difference :-).
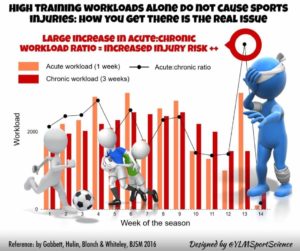
It is 2020 and I still see many runners who have been told to stop running, yet only one had an issue that might improve more rapidly if they stopped running. The others could have continued running.
Given that the emotional/mental and psychological boost from running is such an important side effect that the active runner craves, sidelining a runner should be considered only if absolutely necessary.
For most common overuse injuries, “You need to stop running”… is a phrase I rarely need to use. Often times adjustment to your form, and training loads will suffice. For older runners, understanding they occasionally need an additional recovery day is critical.
Why do many docs recommend that you stop running? Because it is easy for them to say. It is because many do not know the current research or literature. Many might use fear to try and stop you from running. We know that running does not cause arthritis. We know that many runners with arthritis can continue running. Runners need to seek second opinions often.
Even the runner with an arthritic knee can usually still run.
- Runners with knee arthritis should consider more frequent, shorter runs. If you run 30 miles a week, run six 5-mile days instead of three 10 mile days.
- The cartilage in a runner’s knee will usually respond favorably to the low impact, shorter duration repetitive forces.
- Slow down, avoid hills while you are going through a bout of discomfort.
- Build volume (distance) first… if tolerated, then add in speed and hills.
- pain should be mild (3 or less), you should not be limping, and any residual pain should be gone within an hour or two of the end of your run.
Runners should consider and use the following questions when seeking care about overuse injuries.
Should I stop running?
You know as a runner that you do not want to ask this question- because you fear the answer. If the answer is that you should stop running, the next question becomes pertinent.
What could happen if I don’t stop running?
Stress fractures of the hip, tibia or navicular (foot) are three instances where you could do significant harm if you continue running. Having to stop running is rarely needed to calm down most common overuse injuries. Certain injuries would still tolerate cross training. Others still might only require a period of base building or lower intensity runs.
Can we change my running schedule or workouts?
Often times the answer to this is yes. Especially for the novice and elite group. The novice often runs the same pace for each run. It is typically a moderate pace. They do not have long slow runs, nor faster workout days. Elite runners might only be required to cut their mileage, change their intensity and base build for while until their injury calms down.
What other means are necessary to treat this injury and avoid future running injury?
Many injuries can be traced to improper running form eg. not landing with your tibia perpendicular to the ground. Cadence, speed, terrain, and running mechanics are all important variables. Some of you would benefit from seeing a running physio for a proper assessment.
Do you have questions regarding an Orthopedic injury or longevity?
Do you want to talk to an expert who can listen to you for 45-60 minutes and explain the options in detail?
Dr. Howard Luks offers remote guidance sessions to review your X-ray or MRI images and explain your options.
Dr. Luks has also received hundreds of requests for educational sessions on the topics discussed in his book, Longevity Simplified.
Many overuse runners injuries can be traced to a tight achilles, tight hip flexors, poor pelvic control (dip), gluteal and core strength and stability. Often times, while running at a lesser intensity, while working with a physio, athletic trainer or running coach can assist you at getting back to your normal running schedule.
Can I minimize my risks of a running injury going forward?
For the novice, the answer is clearly yes. Consider a few sessions with an online coach or program to design a proper running schedule. These programs also help you add load slowly to minimize the risk of injury. Learn the proper ways to run and how to minimize the risk of injury. Understand the 80/20 rule and the 10% rule and you can dramatically decrease your risk of reinjury. Elites runners function in a zone where maximal performance and overuse injury risk are very close cousins. Their coach will be able to adapt their training schedules moving forward to diminish the acute training load to minimize their risk, the question will be whether or not their chronic training load will also need to be altered.
Bottom line… acute (swollen) , severe pain due to tendinopathy such as achilles tendinosis may require a (very) short rest period. Stress fractures do require a more extended rest. Stress fractures around the hip are a must stop running (may need surgery) severe overuse injury. Other common running overuse injuries might only require subtle changes to your regimen and a better understanding of how runners train.
Many overuse injuries in runners do not require that you stop running. Finding a doc, physio, or athletic trainer that understands the runner’s mentality, and is current on injury detection, and treatment methods are critical if you wish to remain out on the road.








Vicki Le Plastrier
Many thanks Dr Luks. I have a bucket-hole tear which I’ve have been jogging with for at least 7-years (without problems) but it flips / folds from time to time. Never when I’m jogging but rather when I bend my knees to drop down onto the edge of the swimming pool or put my fins on. It is a size-10 pain when I attempt to put weight on it even in the pool. To date, it has eventually resolved itself by simulating the use of my leg as I would to change the clutch in my car. As I’m in Australian I’m unable to visit you surgery so thank you very much for your excellent information. Kind regards
Natasha B.
I know this is an old article, but poignant for me. I’m a 40 yr old woman who was a novice runner for many years. I stopped for awhile and got fat. So I’m back on the treadmill and on a particular day, I experienced a sharp pain in the top of my left tibia. It swelled immediately and I could not walk for 3 days.
It has since dulled, but slightly swells every time I run. The pain is deep and sharp for a day or two after, then it subsides only to return when i get back to the gym,
My PCP refused to send me to a specialist because he said it was due to my weight. (Im about 20lbs over what I should be).
I’m planning on changing my PCP because I think he just doesn’t know any better. My gut tells me it was a real injury that will probably turn into arthritis.
I love running. It is the only exercise tgat slims my legs and gives me a natural high. I dont want to stop. Help!!!!
With immediate pain as well as swelling it is likely an injury that should be evaluated by an Orthopedic Surgeon.
Alice
Thanks for Sharing..
Sue Fine
I lament!! Why aren’t there more doctors like you? Should I travel hundreds of miles to get a doctor who understands me, as a 50-something athlete? I want a doctor who gets this aspect of the mind-body relationship and how it relates to identity, whole person well-being, and treatment plan. I have not been able to find that where I live.
When does it make sense to travel for medical treatment to get whole person needs met? (rhetorical question, but maybe someone does have an answer…)