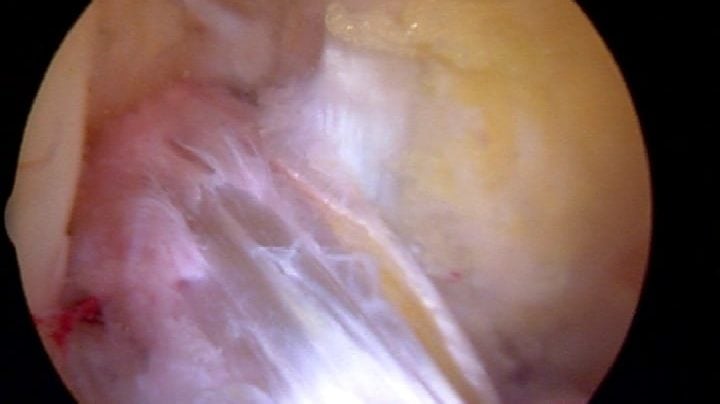
There are many parts that must come together in a cohesive manner to assure the best chance of success following an ACL injury. Those parts include:
- Having a well prepared, well educated and motivated patient. (See ACL Part I and ACL Part II )
- Being under the care of an experienced ACL surgeon.
- Being under the care of a physical therapist who is well voiced in the unique needs of an ACL injured patient.
The success or failure of an ACL reconstruction is not simply determined by placing the ACL properly during the surgical procedure. That is merely one step during a long process that requires meticulous attention to detail. Having an educated and motivated physical therapist in equally as important as executing the ACL surgery properly. Proper physical therapy following ACL injuries is of paramount importance, both before and after your ACL surgery.
I would like to extend a sincere thank you to Julie for sharing this post for our blog. Julie is one of the best educated clinical thinkers in the ACL recovery physical therapy universe. She travels worldwide in search of knowledge and has an extensive history of treating a multitude of professional athletes and weekend warriors alike. Her credentials are listed below and I encourage you to visit her site. I especially encourage those of you involved in the training and care of athletes to download her book on prevention strategies … since an ounce of prevention is worth 10 pounds of cure.
 What patients really need to know about physical therapy and their recovery following an ACL injury?
What patients really need to know about physical therapy and their recovery following an ACL injury?
There are approximately 100,000 ACL tears in the United States each year at a financial cost of $1.7 billion (Silvers, 2014). The number is not decreasing and it is unclear if it is simply because more people are participating in unpredictable activities which involve cutting, pivoting, and jumping or if we are just becoming more prone to injury from lifestyle and environmental factors.
No matter the reason, more injuries are occurring and orthopedic surgeons are busier than ever reconstructing knees of athletes everywhere. Additionally, the risk for a second injury remains high in those who have experienced one and return to sport. “Athletes in the knee and ACL groups were 6.8 and 19.6 times more likely to sustain a knee injury and 14.4 and 892.9 times more likely to undergo a knee surgery during their collegiate careers compared with controls.” (Rugg, Wane, et al; 2014)
Here are a few key messages I wish more people understood regarding their approach and choices for rehab following an ACL injury.
1. An ounce of prevention is worth its weight in gold…almost literally.
There is an ever-growing body of research showing that neuromuscular-based warm-up programs used 10-15 minutes prior to practice/games each week can reduce the incidence of ACL injury by up to 88%. (Mandelbaum, Silvers, et al; 2005) The soccer governing body in New Zealand has implemented mandatory injury prevention program use with all soccer teams in their federation and estimate $8 in health care savings for every $1 invested in prevention. A quick search of researchers such as Ekstrand, Hagglund, Hewitt, Padua, Silvers, and Walden (to name a few) show the real progress we are making in understanding that we can significantly reduce the number of these injuries from happening in the first place. Now we just have to put this knowledge to use; coaches are the #1 barrier to making this happen.
2. What you do before your surgery can make a big difference.
In a 2013 study (Shaarani, et al) on the benefits of prehab prior to ACL surgery, the average time for a return to the sport for those who took part in a prehab program was 34.18 weeks compared to 42.5 weeks for those who went into surgery without participating in prehab. In addition, the prehab time is invaluable for both the physical therapist and patient to build a positive rapport with each other and get to “test drive” how the rehab process might work. Will it be a good fit? Does my physical therapist understand my goals? Does the patient understand my standards?
Three big items in prehab should include:
- Symmetrical range of motion compared to uninjured side
- Minimal to no swelling
- Excellent neuromuscular control and strength of quad.
I typically get patients started on some of the exercises and activities they can expect after surgery in rehab (single leg squats, single leg stabilization activities, functional lifts -not machine based activities, posterior chain work, etc) so they have a chance to learn them prior to surgery. The rehab is about training or retraining the brain as much as the body and this gives them a jumpstart on the brain side of the rehab. It also provides patients with a preview of what to expect in terms of activities and time needed each day to get rehab in. A better understanding of the process leads to better compliance and thus better outcomes.
3. Do your homework on your surgeon and make an informed decision!
Choose a surgeon who does a large volume of ACL reconstructions a year. 85% of orthopedic surgeons do less than 10 per year. (Harner; 2004) You want a surgeon who specializes in this type of surgery and is motivated to stay on top of the latest techniques including anatomical placement of the graft, limiting a number of allografts used in young athletic patients, and trained in using more than just a single type of graft. Above all, you want a surgeon who listens to your goals and places you at the center of the equation. When in doubt, ask a physical therapist who rehabs a lot of ACLs – I often get asked what surgeon I would recommend for ACL surgery based on what I see on daily basis with a wide variety of ACL reconstructions from different surgeons.
4. Do your homework on your physical therapist and choose wisely!
Your physical therapist is the second half of the ACL surgery equation. If the surgery is poor the rehab will suffer; if the rehab is poor – it is a waste of a great surgery. If both are good, the likelihood of a good outcome is high as well. Know that you have the power to choose your physical therapist. It’s your knee, your body and your quality of life – make yourself a priority. Ask around to surgeons and those who have had great rehab experiences what physical therapist they would recommend.
Some things to look for:
- Does your physical therapist understand your sport or activity you are trying to get back to? If they have a pretty limited understanding of what the real physical and mental demands are of your sport and role; find a PT who does (or is willing to put the time in to learn and step into your shoes). In addition, your rehab should be performance-based and in many ways feel like training for your sport (while still respecting graft integrity) once you are out of the immediate post-surgical phase. If it looks strangely similar to your grandfather’s rehab from a total knee replacement you may want to reconsider the direction you are going.
- Does your physical therapist map out the rehab process for you…in specifics? Can they tell you the criteria for moving from one phase of rehab to the next and ultimately what specific competencies you have to demonstrate to determine readiness for full return to competition? ACL rehab is not a cookbook rehab; they shouldn’t be planning your session each day from a book full of protocols. Time from surgery should not be the main determining factor marking your rehab progress; it is a bare minimum guide for the biological healing of the graft only. Your physical therapist should be spending considerable time evaluating how you move in progressively more functional movements – squatting, hopping, lunging, cutting, sprinting, stopping, pivoting…and then again later in an environment that is unpredictable and full of distraction…and related to your sport. A set of body weight squats or wall sits and balancing on one leg with your eyes closed isn’t going to do the job; neither will 3 sets of 10 reps in whatever leg machine of your choice.
- Does your physical therapist take into consideration the psychological component and do they bridge the gap from the clinic to the field? Spending a minimum of 20% of total rehab time on the field/court in competitive athletes is a good starting point for two reasons: Psychologically the athlete will tend to feel more comfortable and find it easier to feel “normal” again; and it also affords the opportunity to put athletes through the full demands of their sport to see how they move in their sport environment while minimizing both the mental and physical gap in performance from the end of rehab to the start of return to competition. In addition, I use an outcome measure/questionnaire during various stages rehab to track how patients are assessing the function of their knee with respect to athletic activities.
- Do not rush back. Does your physical therapist and surgeon communicate? Many people assume they do, but that is often not the case. Paperwork gets stuck on piles, inboxes, etc. The best of both professions will have strong communication channels and use them effectively so the pathway from prehab to surgery to return to competition is smooth for the patient. Don’t assume because they are housed in the same building that communication is happening or that it isn’t simply because they work independently from one another.
70% of ACL injuries are non-contact – meaning the reason you got hurt is most likely a factor of how you move and the compensation you have developed. These don’t happen overnight and don’t resolve overnight either. Just because a certain amount of days has ticked off the calendar and your graft is no longer deemed “fragile” and your quad is strong does it mean you are ready to play. Take the time to overhaul your body and how you move so you don’t find yourself back in the same situation again. The rehab is a marathon, not a sprint. If you do it right and with the right plan, you should be a better overall athlete at the end of it.
Julie Eibensteiner PT, DPT, CSCS is a physical therapist and founder of Laurus Rehab and Performance, an independent physical therapy practice specializing in ACL injuries of competitive athletes in the greater Minneapolis-St. Paul area.
www.laurusrehab.com
Twitter: @laurusrehab
Facebook: www.facebook.com/ACLRehab











Hi dr Luks
It’s Teresa Kasman . I think I would like to try alternative options for my rotator cuff injury. I’m thinking PT, NSAIDS, steroid injections, before surgery . The steroid injection the other day worked amazingly . Therefore it gave me hope on avoiding surgery. What is your opinion?
We should talk in the office