
Derrick Rose Has Knee Surgery to Repair his ACL Tear
As most sports fans know… both Derrick Rose and Mariano Rivera recently sustained ACL tears. The ACL is the anterior cruciate ligament and for those interested, this short knee anatomy video will show you the structure of the knee, and more specifically the ACL.
After a course of “pre-habilitation” Derrick Rose recently underwent surgery to repair his ACL. The Chicago news media reported that the surgeon chose a patella tendon graft and also elected to perform a PRP or Platelet Rich Plasma injection at the time of the surgery. Let’s look at these aspects of his ACL surgery and events leading up to it more closely.
Rehabilitation Before Surgery:
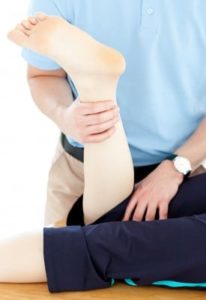
Most surgeons recognize the benefit of pre-hab or physical therapy before surgery. The focus of pre-hab is to:
- Allow for the swelling to subside
- Decrease the inflammation within the knee
- Let you get back some of the lost strength in the muscles supporting the knee.
A more flexible, less painful knee before ACL knee surgery, leads to less swelling, less inflammation and hopefully an easier recovery after ligament surgery for an ACL tear.
 Graft Choices for an ACL Ligament Reconstruction:
Graft Choices for an ACL Ligament Reconstruction:
As surgeons we have many graft choices available to reconstruct or rebuild your ACL tear. These include:
Autografts (your own tissue):
- Hamstring Tendons: Where we use two (of four) of your tendons to create the new ACL.
- Quadriceps Tendon: Where we take a portion of your quadriceps tendon (above the kneecap)
- Patella Tendon: Where we take the central ⅓ of your patella tendon (below your kneecap)
Allograft: (Cadaveric tissue, or tissue from someone who has passed on and donated their tissues for medical use)
- Patella Tendon
- Quadriceps Tendon
- Achilles Tendon
- Hamstring Tendons
- Other tendons from the leg
The most important factor is not necessarily which tissue you chose to use for your ACL reconstruction eg: patella tendon vs. hamstring tendons. The bigger decision is whether or not to use autograft or your own tissue, versus allograft, which is from a cadaver. There is recent scientific literature which reveals a higher re-tear rate in children if an allograft is used versus autograft.
PRP or Platelet Rich Plasma:
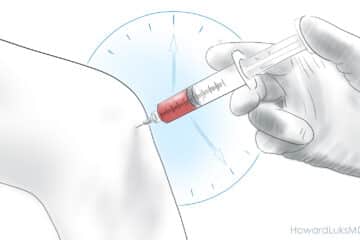
PRP, or platelet rich plasma is a portion of your blood that we prepare by taking a sample of your blood, approximately 30-60cc, and then that blood is placed in a centrifuge for 15 minutes. After that the blood separates into different layers or components. One of those layers contains the platelets, which are cells which contains a number of growth factors and chemicals which initiate a reaction by the body to repair the area where the platelets are.
PRP has proven to be useful in the treatment of tennis elbow, and other tendon related disorders. PRP is also being actively investigated to determine if it is useful in improving the healing time after surgery. While PRP is a well accepted treatment for certain tendon or muscle problems and has become very popular, there is less certainty as to whether or not it is useful when used at the time of surgery.
Hopefully Derrick Rose continues to recover well from his recent ACL reconstruction!
Do you have questions regarding an Orthopedic injury or longevity?
Do you want to talk to an expert who can listen to you for 45-60 minutes and explain the options in detail?
Dr. Howard Luks offers remote guidance sessions to review your X-ray or MRI images and explain your options.
Dr. Luks has also received hundreds of requests for educational sessions on the topics discussed in his book, Longevity Simplified.
 Graft Choices for an ACL Ligament Reconstruction:
Graft Choices for an ACL Ligament Reconstruction:





Fabien
Hi Dr Howar,
I am wondering if you could comment on my surgery report for knee reco.Here are the details. My big issue is that i have 3 vertical longitudinal partial thickness tears and that I am really worry about risk of OA in the future. I would appreciate if you could let me know your professional opinion on my situation. I am 43 and going forward will mainly be cycling, do some strengthning gym work and skiing (2 weeks a year). Should I be worrying about anything in particular from this report ? Are these tears likely to propagate ? I am also active ; 1.82 and 88 kg.
I have copied at the end of this report the questions I am currently planning to ask my surgeon when I see him for the 4 months follow up exam next monday. Please let me know if there are other questions I could ask.
Thanks again for all your time spent on this forum.
Fabien
Examination Under Anaesthesia:
No effusion. 0 Recurvatum to 140 flexion. Lacham 1+ with an equivocal end point. Pivot shift 2+. No collateral laxity
Operative procedure
A tourniquet was applied and anthroscopy performed using anterolateral and anteromedial portals. No abnormality was seen in the patellofemoral compartment. In the medial compartment the articular surface was intact. Probing revealed an inferior surface partial thickness vertical longitudinal tear on the inferior surface of the posterior horn of the medial meniscus. The tear was very peripheral and was approximately 12 mm in length. As it was stable, it was felt that there was little to be gained by trying to suture it, given the patient’s age. In the intercondylar notch there was a proximal rupture of the anterior cruciate ligament. In the lateral compartment the articular cartilage was intact. There were small inferior surface and superior surface partial thickness vertical longitudinal tears on the posterior horn of the lateral meniscus . These were stable and were not addressed surgically.
Main priorities:
• Delaying onset of OA
• Return to skiing (2 weeks per year)
1.
2. Is there a chance that my meniscal tears can heal by themselves (maybe due to the bleeding in the knee joint during the ACL reconstruction or location of the tear )
3. What is the impact of each of the meniscus tears on my knee ?
4. Is it likely that any of the 3 meniscus tears will propagate without re – injury ? Is there a way to prevent that ?
5. What is the impact of each tears on my knee ? Do I need to avoid any activities ?
6. Is PRP an option with regards to fixing the meniscus tears and trying to restore its functionality ?
7. From your experience how high are my risks of longer term OA and knee replacement due to these injuries and how can I delay onset of knee OA? ( I don’t have any family history of knee OA).
HI again Fabien … I’m sorry. I can not comment.