
SLAP lesions are a unique type of labral tear in the shoulder. SLAP lesions occur in overhead athletes due to chronic repetitive stress. But many SLAP lesions are simply due to aging. How should your SLAP lesion be treated? MRI machines have become more powerful and radiologists have become better at interpreting the findings. Perhaps that is why shoulder surgeons have noticed a significant increase in the number of SLAP lesions being diagnosed across all age groups. It is important to bear in the mind the research of DePalma performed over 70 years ago. During his autopsy studies, he found that more than 75% of people over 60 had labral tears in the shoulder. Simply stated that means that the majority of these tears are not bothersome, do not hurt you and thus do not, in and of themselves require surgery. Again, as hard as it is to hear, sometimes our parts simply wear out. So it is important that we listen to you describe your symptoms, correlate that with a proper physical exam and then determine if a SLAP lesion is the cause of your pain.
What is a SLAP lesion or SLAP tear?
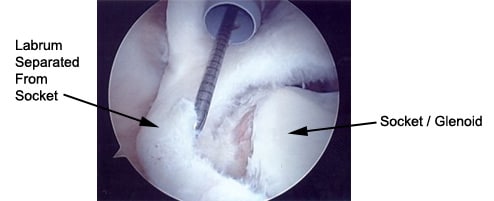
The two terms are synonymous. They mean the same thing. As the picture above shows, a SLAP lesion involves the tear of the glenoid labrum from the top of the socket of the shoulder.
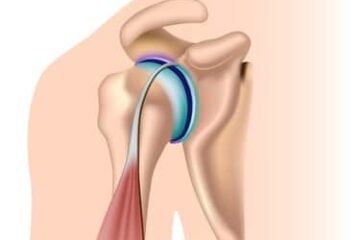
The superior labrum serves as the attachment for our biceps tendon inside the shoulder. The labrum plays a role in the stability of the shoulder. It helps keep the shoulder well seated within the socket during aggressive overhead activities such as pitching, swimming and playing volleyball. The superior labrum does not come into play from a functional perspective during our normal daily activities of dressing, feeding, cleaning, weeding, gardening, running, cycling, etc.
Why do SLAP lesions hurt?
SLAP lesions can lead to a unique form of instability (where the shoulder is “loose”), and as previously mentioned, primarily occurs in overhead athletes. When the shoulder is loose because of a SLAP tear, and the player puts their arm up in the throwing position they may feel pain in the back of the shoulder. We call this “internal impingement”. This occurs because the SLAP tear has led to a very subtle loosening (not enough for the shoulder to dislocate) which will hurt when the superior labrum (where the tear is) is stressed.
Does a SLAP Lesion require surgery?
A troubling study was just released …
A study in May 2012 issue of The American Journal of Sports Medicine reflects this trend (towards operating on too many SLAP tear). Alan L. Zhang et al looked at insurance data collected for over 11 million patients from 2004 to 2009. They found a remarkable 105% increase in SLAP repairs performed across the United States between 2004 and 2009.
The 20-29 year and 40-49 year age groups had the highest incidence of SLAP repairs. Males comprised approximately 75% of those surgical patients. Interestingly, SLAP repairs were performed more often in the West and the South compared to the Midwest and Northeast.
The majority of SLAP lesions or tears encountered in a typical orthopedists office do not need to be repaired and are usually not the source of pain. Even if the surgeon believes that the tear might be the source of pain, the results of repairing SLAP lesions has been relatively poor in patients over 35-40, so many researchers suggest that the tear not be fixed and that a biceps tenodesis be performed ( anchoring the biceps on the humerus and taking the stress off of the superior labrum.
SLAP lesions found in young pitchers, volleyball players, tennis players and swimmers can be fixed if the tear is leading to significant pain and the inability of the athlete to perform at their usual performance level. They do, however, have the option of changing positions, etc and not having surgery. But bear in mind, just because a SLAP lesion is fixed, does not mean you will return to pitching.
The results of SLAP lesion repairs and return to sports is also mixed. Some reports show that athletes can return to their prior performance levels, yet some recent literature shows that that might not be the case. The jury is still out on this.
Bottom line:
SLAP lesions are very common. Just because you have one, does not mean you need surgery. If you are an overhead athlete and have internal impingement due to a SLAP tear you may choose to have surgery – but you may not be able to return to your prior level of functional performance. Tough decision.










I am a 16 year girl. I have undergone MRI test. Will it do me wrong in the future.
The MRI will not hurt you … Cat Scans can.. not MRIs
I am concerned about my 50 year old relative. He complained of pain in his shoulder two monthsago; it went away then returned days later when he wasdriving. He has been going to work in manufacturing job where he has limited his own lifting and has not missed any work. He went to his doctor, got an MRI (I am not a doctor, but the language sounded like minor concerns) He was then sent to a surgeon and was told because he is a young man he needs surgery right away to repair the tear instead to removing the muscle. Below is what the MRI and surgeon notes state. I want him to get another opinion before surgery because I am worried the surgery will make his disabled and unable to work again.I kinda think this is something that heals itself and takes time, but does go away. What do you think?
Findings:
• Only mild changes of osteoarthritis at the acromioclavicular joint, but the joint capsule is markedly thickening and fibrotic. There is no subluxation or erosion. The acromion is mildly laterally downsloping.
• There is trace fluid in the subacromial/subdeltoid bursa
• The supraspinatus, infraspinatus and subscupularis tendons are moderately thickened and contain heterogeneous increased PD and T2 signal, but no descrete tear is apparent. Only the teres minor tendon is normal.
• The rotator cuff muscles are unremarkable, with no edema or atrophy
• The glenoid labrum is within normal limits on this study without intra-articular contrast.
• The long head biceps tendon is markedly thickened and is of increased PD and T2 signal intra-articularly, but no discrete tear is apparent.
• Glenohumeral articular cartilage appears well-preserved.
• Contours of humeral head and glenoid rim are normal.
• There is no glenohumeral subluxation,
• There is a trace glenohumeral joint effusion
• No loose body is apparent.
• There is no periarticular fluid collection.
• There is no evidence of fracture, avascular necrosis, or destructive osseous lesion.
MRI Conclusion:
1. Moderate tendinopathy of supraspinatus, infraspinatus and subscupularis and long head biceps tendons
2. Trace glenohumeral joint effusion and trace fluid in the subacromial/subdeltoid bursa
3. Only mild changes of osteoarthritis at the acromioclavicular joint, but the joint capsule is markedly thickening and fibrotic.
4. Full range of motion. Tenderness with palpation subcaosular bursa posteriorly. Point tenderness over biceps tendon. Increased pain with resisted flexion and supraspinatus isolation. Pain with range of motion, no instability.
His doctor sent him to an orthopedic surgeon:
Exam note: Full range of motion. Tenderness with palpation subcaosular bursa posteriorly. Point tenderness over biceps tendon. Increased pain with resisted flexion and supraspinatus isolation. Pain with range of motion, no instability.
Diagnosis: SLAP tear, degenerative in nature vs primary buceps tendons partial tear or tendosynovitis. Left shoulder subcapsular byrsitis
Surgery: Left shoulder arthoscopy with SLAP repair and bicep debridement or tenotomy.Will inject subcapsular bursa at same time
There is noting on the MRI that requires surgery. We do not fix SLAP lesions in 50 year olds. If he is working and comfortable he should continue working :-)
Besides… even if he has some residual pain, it would not be treated with a SLAP repair at his age. And it is NOT an urgent matter.
Thanks
Hi Dr. Luks,
I’m a 25 year old male. 3 years ago I had a hard fall on an outstretched arm, that had me in a lot of pain at the time. It subsequently got better – and currently I only feel a very moderate amount of (dull) pain, which feels slightly worse after using the arm for a bit. I have full ROM. This pain and the fear of doing further damage makes me avoid using my arm for anything too strenuous.
I recently got diagnosed with detachment of the superior labrum/biceps anchor inferiorly – consistent with a SLAP type 5 injury and possible small bony Bankart lesion, and thickening/oedema and inhomogeneity of the distal infraspinatus (IS) tendon mainly at its anteromedial/articular surface extending from 10mm proximal to and directly onto its postero-superior greater tuberosity attachment consistent with partial thickness articular surface tear/chronic tendinosis / tendinitis.”
My doctor is recommending surgery.
I would just like to find out if physical therapy may be worth a try first?
I am worried that the risk and length of recovery from surgery may not be worthwhile as the pain is manageable. Although I also don’t want the tear to get any worse, or to restrict the use of my arm too much in the future.
Thank you so much!
Donald
So… SLAP lesions only need to be treated surgically if the pain is interfering with your quality of life. If your shoulder is not dislocating then it’s not typical to consider surgery for a Bankart lesion.
This is your call … and your choice… and the choice should be made depending on how much pain you have… not because you have something torn. Many people are walking around with a SLAP lesions and lead very active happy lives.
Good luck !
Hi Dr. Luks,
I had a biceps tenodesis and subacromial decompression in 2012 after a fall in an exercise class the previous year led to SLAP and biceps tears. Pain returned in five weeks ago after being low or non-existent for many months. The pain started a day after pumping bicycle tires, although I had no pain while pumping the tires. I have started in recent days to take naproxen 500 mg/day, but this has not helped yet. Most of the pain is in the posterior shoulder and is often constant, even at rest and often worsens as the day goes on. I have had a few flare-ups over the past couple of years, but they have lasted only around 7 to 10 days. This flare-up has lasted more than a month with no end in sight. Suggestions? Thank you!