Osteoarthritis is usually not a mechanical wear and tear process. If you have osteoarthritis, exercise will not wear out your knee joints faster — quite the opposite. Knee arthritis exercises have been shown to relieve the pain of mild knee arthritis and does not harm the cartilage. This post will dive deep into the science to support why we should start knee arthritis exercises to improve knee pain associated with osteoarthritis. This post will also offer other tips and pearls to improve your knee arthritis pain.
For those of you who prefer a podcast format, here you go.
How many of you have been told to rest and stop running or exercising because you have knee arthritis? Far too many people believe that arthritis is caused by mechanical wear and tear. It’s only natural that you might assume that your arthritic knee pain will worsen with exercise. Too many health care professionals counsel their patients to stop running, speed walking, elliptical, treadmill, etc. to “save” their joints. Most of the time, you need to do just the opposite. The research over the years has been unequivocal.
Running may improve cartilage nutrition
Exercise has been proven to be the most effective treatment for early and moderate osteoarthritis of our joints. Exercise improves all-cause mortality and decreases your risks associated with muscle loss, frailty, sarcopenia, and so on. We are going to walk through the current research and evidence-based recommendations for the management of arthritic knee pain.
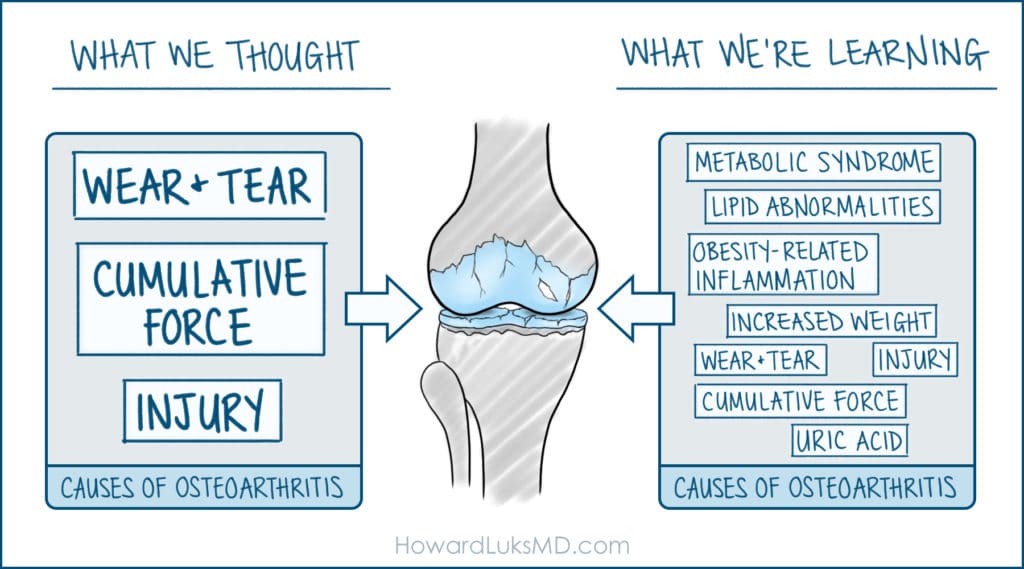
What are the causes of osteoarthritis of the knee?
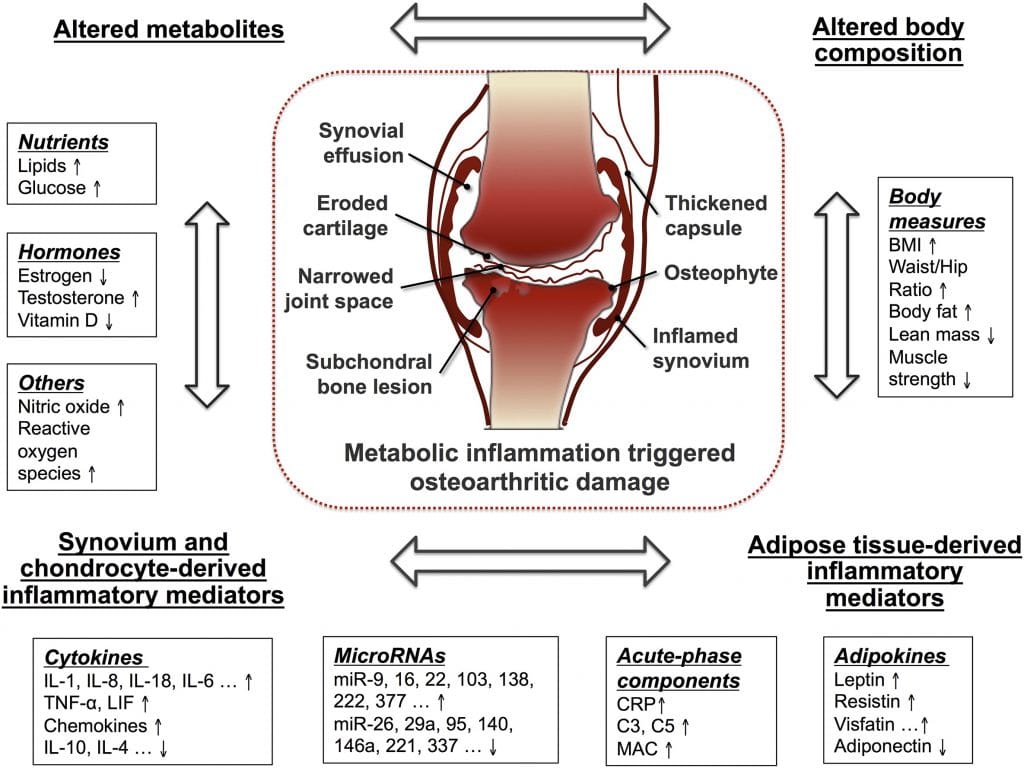
What is arthritis in the knee? Let’s start at a very basic level. There are many potential causes of osteoarthritis of the knee. In people without prior injuries osteoarthritis is usually a biologically mediated inflammatory process…. what does that mean?!?
In our joints, we have 100s of proteins, cytokines, chemicals, and other compounds which are made by the synovium, or the lining of the knee joint. When our joints are healthy, the chemicals in our joints support cartilage health and nutrition.
Whether it is due to injury, or our metabolism, weight, and diet — a switch flips. Changes occur in our knee joint that is similar to the changes associated with other chronic disease states. That switch turns on genes in our DNA that increase the production chemicals that are hostile to the health of our cartilage. So over time, an increase in those unfriendly chemicals eventually causes cartilage cell injury. The cartilage is the cushioning in the knee that protects the knee from developing knee arthritis. That weakens the cartilage and its ability to withstand stress.
If the cartilage is not functioning well, or if it becomes thinner, it can lead to pain, inflammation, warmth, and swelling. Osteoarthritis appears to be caused by low-grade chronic inflammation. This is the same chronic inflammation held as a cause of other chronic diseases such as Type 2 diabetes, heart disease, and fatty liver.
Much of the chronic disease burden that affects us appears to have a metabolic etiology or cause. A few months ago, we discussed the issue of metabolic health and its impact on our health in this post. We also discussed how chronic inflammation could lead to diseases, including dementia and heart disease.
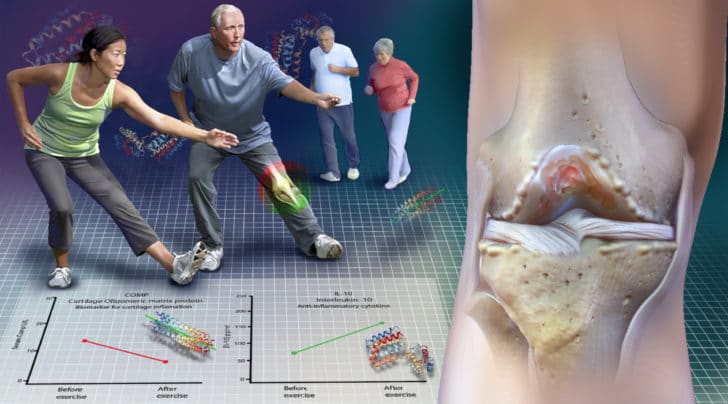
Researchers are determining how all these proteins and substances in our knee joint affect cartilage health and the incidence of osteoarthritis. Exercise has been proven to decrease the concentration of proteins and compounds in our knees that are hostile to cartilage health.
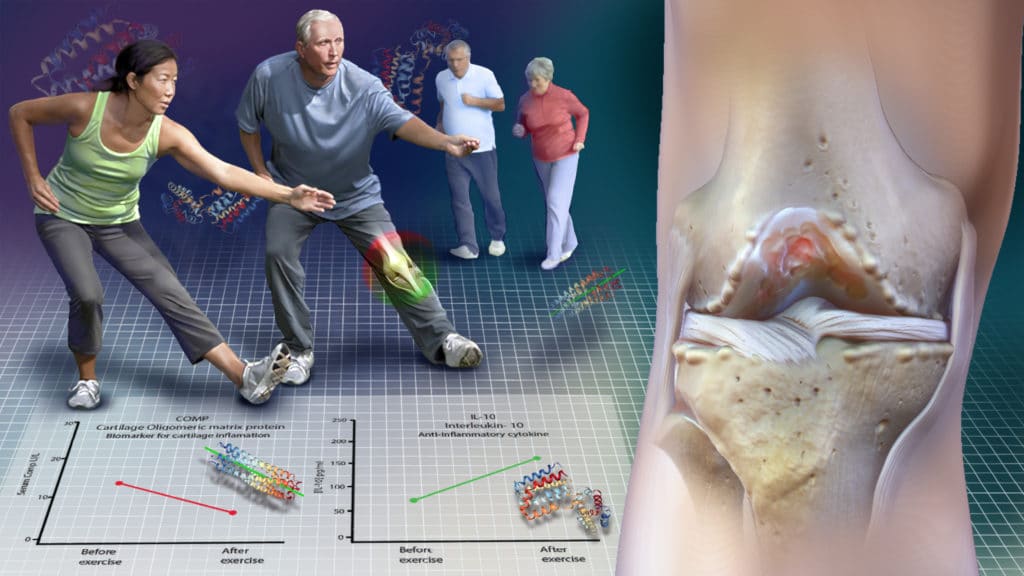
In this study, IL-10, a cartilage protective chemical in the knee, was produced in response to exercise. Also, the concentration of a compound called COMP decreased within the knee with exercise. COMP is a protein that is felt to be a biomarker of cartilage degeneration. This study shows that COMP levels in the blood increase during exercise but quickly return to baseline. The increase in COMP in the blood does not seem to reflect a negative effect on an arthritic knee.
Other research studies show that the concentration of COMP within the knee decreases with exercise. Therefore, exercise might cause the COMP within the knee to be pushed into the bloodstream, or the lymphatic system with activity. Decreased COMP within in the knee, combined with an increase in the concentration of Interleukin-10 appears to show that exercise is not harmful to cartilage, and may be beneficial. This research shows that running was associated with a decrease in the cytokines or the chemicals in the knee related to cartilage wear and degradation.
Yes, there are mechanical causes of osteoarthritis. People with severely bowed knees or knock knees are more prone to developing arthritis. That’s because you are overloading one side of the knee joint if your knee is mal-aligned. If you had a meniscus removed because of a tear, you are also at an increased risk of developing osteoarthritis. Certain fractures or broken bones that involve the knee joint can lead to post-traumatic osteoarthritis. Post-traumatic arthritis is rare, and it is due to the injury’s subsequent mal-alignment after the fracture heals.
Common knee arthritis symptoms?
In other words, what does arthritis in the knee feel like?
The signs of knee arthritis can vary significantly. With mild arthritis, many people will have an ache associated with walking, stairs, or running. The location of the ache or pain can be on the inner side of your knee, the outer side, or even in the back of the knee.
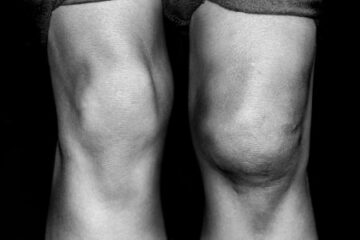
Osteoarthritis in some people will produce swelling, or what is commonly referred to as “water on the knee.” Therefore some of you may have swelling of the knee while others will not. Depending on the location of arthritis within your knee, it can feel like it wants to give way.
Some people with knee arthritis will have the feeling that the knee is unstable, or that the knee will not support them. Some people with that feeling will notice an improvement if they use a compression knee sleeve. Simple compression sleeves might work well. Sometimes you need a knee arthritis brace with more support.
A feeling of griding or “crepitus” is a common complaint. When the inflammation due to knee arthritis increases, you may have knee pain at night. That’s why you may reach for a pillow to put between your knees when you sleep. Morning stiffness of the knee, or stiffness if you have been sitting for a while is a common complaint if you have inflammation associated with knee joint cartilage degeneration.
So, the most common symptoms of knee arthritis are:
- swelling
- achiness
- occasional sharp stabbing pain
- grinding or “crepitus”
- a feeling that the knee is not stable.
- knee giving way
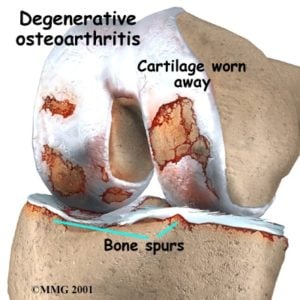
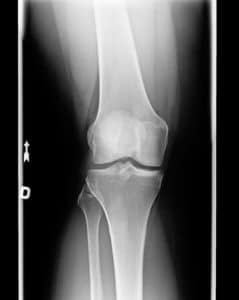
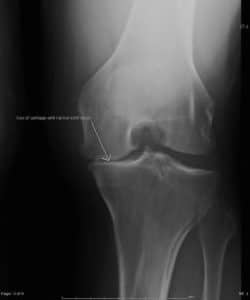
What does knee arthritis look like on X-ray?
The cause of knee arthritis is not entirely clear. Very different clinical pictures emerge when we see people in our offices and clinics. Some of you have mild arthritis that does not bother you much. Arthritis might progress or worsen slowly over decades, or it might progress more rapidly. In some, the pain you have might be minimal, and in others, the pain might be severe, regardless of how your X-rays look. That means that we have some patients with mild arthritis on an Xray, but they have severe pain and swelling. Others might have only a little pain despite X-rays that show severe arthritic changes.
Metabolic Health and Knee Arthritis
The burden of osteoarthritis has been increasing across the globe. This is similar to the increase in chronic diseases such as dementia, high blood pressure, Type 2 Diabetes, and heart disease. All of the tissues in our body, including our cartilage, are sensitive to our dietary intake. Metabolic issues are felt to have a causative role in the development of osteoarthritis and other chronic disease states. The earlier in our life that we realize this, the better off we will be.
This post goes into more detail about the effect of our diet on our joint health and overall health. What might cause those genes in our DNA to become active? Good question… It may be coded in your DNA. So if your parents have osteoarthritis your risk for getting it is higher. Like other chronic diseases you have heard me talk about, OA is similar in that it may be caused by poor metabolic health. It may also have been caused by an injury that occurred 20 years ago. One bleeding episode in the knee can initiate the process. Surgery can start an arthritic process too. Having a meniscus tear, and certainly having that tear removed compounds the problem. That adds a mechanical issue to the inflammatory biological issues- the perfect storm for OA and a good reason to avoid meniscus surgery if you can.
Individual experiments have proven that the concentration of those nasty chemicals in our knee will go down after running, or resistive exercise. Studies have also shown that the health of our cartilage is positively affected by running. Our cartilage seems to like the cyclical loading associated with certain activities. Most studies have shown that the chemical composition of cartilage is not adversely affected by exercise while many studies show that knee pain from arthritis improves with exercise, the exact reason why is yet unclear.
Can I exercise with arthritis of the knee?
 For more than two decades, the research has clearly shown that exercise is of benefit in people with osteoarthritis of the knee. Exercise improves pain, strength, and decreases muscle atrophy. Exercise can improve your quality of life and help delay the need for surgery. So.. if someone tells you to rest because you have osteoarthritis… kindly say no.
For more than two decades, the research has clearly shown that exercise is of benefit in people with osteoarthritis of the knee. Exercise improves pain, strength, and decreases muscle atrophy. Exercise can improve your quality of life and help delay the need for surgery. So.. if someone tells you to rest because you have osteoarthritis… kindly say no.
Osteoarthritis is not caused by walking too much or low-impact activities. If your arthritis pain is due to severe osteoarthritis, then you may need to consider other treatments above and beyond exercise. Exercise has significant anti-inflammatory effects. This is somewhat counter-intuitive, and I often have difficulty convincing people of this. That’s because far too many people still think the knee arthritis has a wear and tear etiology. The benefits of exercise are enormous. There are more than a dozen chronic disease states that will improve if your exercise. Most of you will feel better if you exercise. The reasons for this are complex, but the results are straightforward. You will be healthier, lighter, feel better, and often have less pain if you exercise regularly—even with mild to moderate osteoarthritis of the knee.
A proper exercise program to combat the age-related changes that we all experience will include aerobic exercise (walking, running, biking, swimming, etc.), resistance exercise, and balance exercises. These different forms of exercise help minimize the risk of developing age-related muscle loss (sarcopenia), heart disease, dementia, type 2 diabetes, hypertension, and so on. This post on our site goes into more detail about the specific exercise programs we should be interested in to optimize our lives for a longer healthspan.
These two posts on my site go into detail about:
1. How muscle mass and muscle strength affect longevity and
2. 6 reasons why you should perform mostly leg exercises.
How does exercise improve knee pain due to arthritis?
The answer to this is much more complicated than you may think. We feel pain in our joints for many reasons. Osteoarthritis of the knee is an inflammatory process. We have proteins and chemicals in our knee joint that our body produces. There are many of these chemicals.
In sedentary individuals who have the fluid in their knee tested and compared to those of us who are active, we start to see significant differences in the make-up of the chemical milieu that is in our knee joint. For example… IL-10 is an anti-inflammatory that our own body manufactures inside our knee joint. After exercise, either resistance exercise or aerobic exercise, the concentration of IL-10 increases.
The concentration of IL-6, a pro-inflammatory mediator, increases with sedentary behavior. For those of you who have arthritis, you knew this already. You know how the first few steps you take in the mornings are tough, you’re stiff, and your knee joint hurts. Well, you have been sedentary, so pro-inflammatory mediators have built up. Now you start walking, and your joints begin to loosen up and feel better. That’s because your anti-inflammatory mediators are beginning to be manufactured.
People with arthritis in the knee want pain relief.
If you have read this far you have a far better understanding of knee arthritis. But knee arthritis hurts, and you need to know some ways to achieve knee arthritis pain relief.
Now, there are short term things to do to help with your knee pain, and then there are long term measures to improve your knee arthritis pain.
In the short term, many of our patients report relief of their knee arthritis pain with one or a combination of the following: Many home remedies for knee arthritis pain are included in this list.
- Moist heat. A heating pad or a warm bath. Some of you may prefer ice… that fine, but heat often works best.
- Tylenol. If you are healthy and of an average size Tylenol should be taken 1000mg every 8 hours, or three times a day.
- Capsaicin: Capsaicin is an ointment. It can work well for knee arthritis pain. Capsaicin is one of the most studied home remedies for knee arthritis pain. But you need to use it as directed on the package. It needs to be applied often for it to work best. Caution: capsaicin can cause burns in some people, so be careful and test small areas first.
- KT tape: Many people with knee arthritis pain will benefit from taping their knee. This tape is available online, and there are many videos to show you how to apply it. Your physical therapist can assist you with proper knee arthritis taping techniques too.
- Compression sleeves: Compression sleeves help minimize knee arthritis pain for many people. We put up a post a while ago about some of the compression sleeves that our patients like. Compression sleeves and other types of knee arthritis braces can help with knee arthritis pain and knee arthritis instability when your knee feels wobbly or you fear that your knee will give way.
- Cosamin DS: Many people report that their arthritic knee pain diminishes when they use glucosamine and chondroitin sulfate.
- Omega-3 Fish Oils: Fish oils have significant anti-inflammatory properties. It can take weeks for the fish oils to start to work. Many of our patients with knee arthritis pain feel better taking fish oils as an anti-inflammatory. You need to continue it for nearly 2 months before you conclude that it is, or isn’t working for you.
Long-term:
- Exercise: during the rest of this post we will discuss why exercise is important if you have knee arthritis. We will discuss why exercise makes knee arthritis pain feel better. Usually, there are very few exercises to avoid with knee arthritis. Exercise will not worsen the arthritic changes inside your knee. If you start an exercise program, your knee arthritis pain might increase for the first few weeks. That’s because these knees can be cranky. Don’t despair. It usually gets better.
What types of exercise should you do for knee arthritis?
If you have knee arthritis, the best exercises you can do are aerobic, balance, and resistance exercises. Aerobic exercise for knee arthritis can be as simple as walking. You do not need to walk 10,000 steps a day. Walking is often tolerated well by people with mild or moderate knee arthritis. If walking is too bothersome, then try an elliptical machine or an exercise bicycle.
Balance training is critical. People with knee arthritis often feel as if they are going to fall. That feeling can be due to pain, or it can be due to a loss of balance. We need to train balance just like we need to train muscles. Simply standing in the kitchen, lightly hold the counter, and lift one leg in the air. Do you feel stable? If not, continue to support yourself by holding onto the counter. Once you feel secure, you can let go of the counter. You should be able to stand with one leg in the air for 15-30 seconds without having to put your other foot back down. Now repeat this with the other leg.
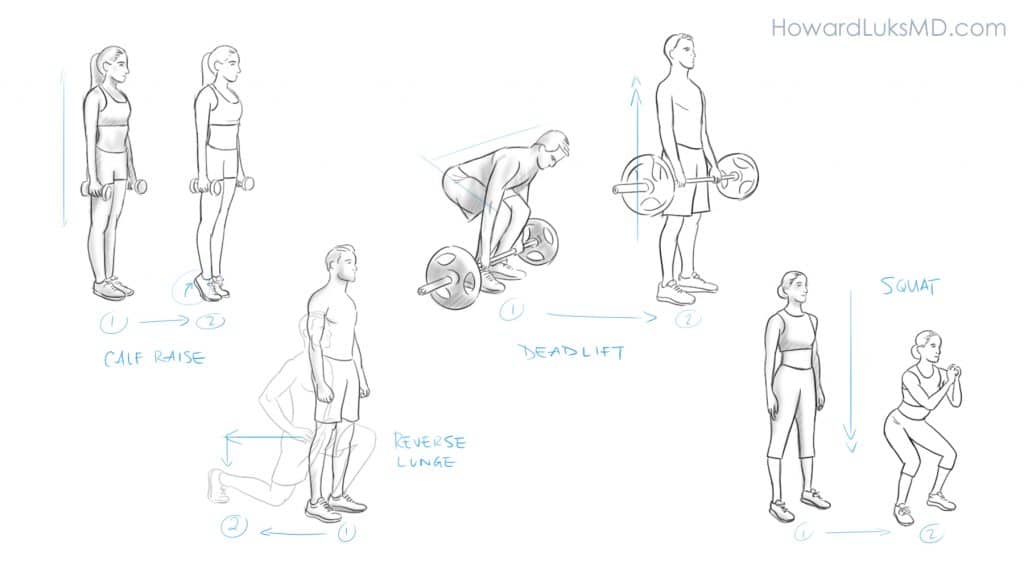
Resistance exercises are also critical for people with knee arthritis. These knee arthritis exercises will increase your strength. It will make it easier to get off the floor, out of a chair, and get up and down the stairs. If you tolerate various resistance exercises then there really aren’t exercises to avoid with knee arthritis. Chair squats, where you sit in a chair and stand are a great start. Hopefully, you can do these without using your arms for assistance. If you need your arms to help, that’s fine. Just keep up with this exercise until you no longer need to use your arms to help push you up.
Working with a professional such as a Physical Therapist or Athletic Trainer is also important. They can assess you and provide you with a set of knee arthritis exercises that you can then do on your own once you learn the proper form.
Running and arthritis of the knee
Far too many people still believe that running causes arthritis and knee joint deterioration. Recreational running, even those of us who have been running 20 miles a week for 40 years has not been associated with an increased risk of developing osteoarthritis. Study after study reveals there is no conclusive evidence that running causes osteoarthritis of the knee; in fact, running may actually slow the functional aspects of musculoskeletal aging. Various initiatives have evaluated the risk of developing arthritis or the risk of worsening osteoarthritis of the knee in runners. There is no conclusive evidence to suggest that running is going to cause arthritis to worsen. We published a few posts on this website on the topic of running with osteoarthritis and meniscus tears. Feel free to dive deeper by reading those posts.
The importance of knee arthritis exercises
For most people, aerobic activity as a knee arthritis treatment is associated with less knee arthritis pain and less disability.
Runners are particularly sad when diagnosed with knee arthritis. Running has not been shown to cause more advanced osteoarthritis. Even as far back as 1986 early studies on runners showed that their bone density increased (that’s good) and there were no signs of increasing osteoarthritis in male or female runners. Like other aerobic forms of exercise. There are numerous health advantages to running. For now, it appears very clear that the risk of not performing aerobic exercise is much higher than the risk of causing worsening arthritic pain.
Osteoarthritis of the knee is associated with an increased risk of all-cause mortality. That means that exercise and maintaining physical activity is critically important for your health and well-being. Formal programs are starting to emerge across the globe to help people improve their quality of life with arthritis that is not yet severe enough to require joint replacement surgery. GLA (D) is a program developed in Denmark that has demonstrated significant success in mitigating a lot of the disabling aspects of living with osteoarthritis of the knee. Exercise and walking are essential to decrease the risk of dementia, lower the risk of heart disease, maintain or decrease our weight, clear the cobwebs from our heads, reduce blood pressure and improve our overall health. Exercise is the best medicine for a joint that has started to degenerate or become arthritic. You are NOT wearing out your cartilage by walking or running.









So, reading between the lines, we should encourage our patients to engage in exercise, despite the pain that accompanies the effort/load of the exercise, correct?
Am I on track to tell patient’s that if the “same” effort/load is accompanied by increasing intensity of pain, as a trend over time (days), they should reduce the effort/load? And, if “same” effort/load is accompanied by decreasing pain intensity, they should increase the effort/load?
Thanks for your guidance.
Joel Dykstra PT, Cert MDT
Evanston Illinois
HI Joel..
I do think that pain can be a useful guide– with some caveats. During the first 2-3 week acclimatization phase I tell folks that they may experience a short-lived increase in symptoms. Their joints are getting used to the load, etc. Following that, I think the most important message, and one that resonates with the majority of OA patients in the office is that there is no evidence that the discomfort correlates with an increase in OA changes or OA progression. Most are comforted by that last statement and most are happy that they can continue to walk, bike, exercise, etc without fear of harming themselves. It almost seems as if their discomfort is better tolerated when coupled with the knowledge that it does not appear that they are harming themselves. The benefits of exercise – aerobic, resistance, and balance- clearly outweigh any risk there might be in continuing to exercise.
Very good info indeed.!It is very very useful atmany points it vanishes the age-old beliefs about knee pain.