Degenerative meniscus tears are very common. Many adults over 55 have one and will not know it. Surgery for degenerative meniscus tears is rarely necessary. Most research shows that people do just as well with physical therapy. This post will carry two messages, both equally important. First, surgery is rarely necessary for degenerative meniscus tears. Perhaps even more important is that once your knee feels better, and it may take several months, you should try to return to your normal activities.
Think about this second statement for a moment. If you had an episode of knee pain, and you had an MRI which revealed a degenerative tear; even though you now feel better you may not return to being active because you are afraid of harming your knee. Arthritis and other conditions worsen, even if you are at bed rest. Meniscus degeneration and tearing are no different. It is more of a biological issue than a mechanical issue. Meaning that you cannot stop the process, so you might as well remain active.
Why would you want to slow down your activities which are decreasing your risk of diabetes, obesity, dementia, hypertension, heart disease, and stroke? Rest comes with a heavy burden with respect to your overall health.
Recent research about degenerative meniscus tears and surgery:
The meniscus is a cushion inside your knee. It aids in the stability of the knee and minimizing the stress across the knee, thus minimizing the risk of developing osteoarthritis.
Meniscus tears are incredibly common. Although meniscus tears occur in all age groups, they are most common in adults over 55. There are many different types of meniscus tears. By far the most common tear is a degenerative tear of the posterior horn of the medial meniscus.
An article published in the New England Journal of Medicine out of Finland studied patients with degenerative meniscus tears. They studied whether the results of an arthroscopy (surgery) was better than a sham surgery (where the patient is brought to the operating room and thinks they had the surgery).
As published in the NY Times, The authors found …
A popular surgical procedure (arthroscopy) worked no better than fake operations in helping people with one type of common knee problem (degenerative meniscus tear), suggesting that thousands of people may be undergoing unnecessary surgery.
The Wall Street Journal posted a similar article, and led off by saying…
A fake surgical procedure is just as good as real surgery at reducing pain and other symptoms in some patients suffering from torn knee cartilage
These findings are not new, but in this environment perhaps they will shine a light on the over-treatment of degenerative meniscus tears. In 2007 a study showed that the results from an arthroscopy for a degenerative meniscus tear were not superior to a supervised exercise program.
What is a degenerative meniscus tear?
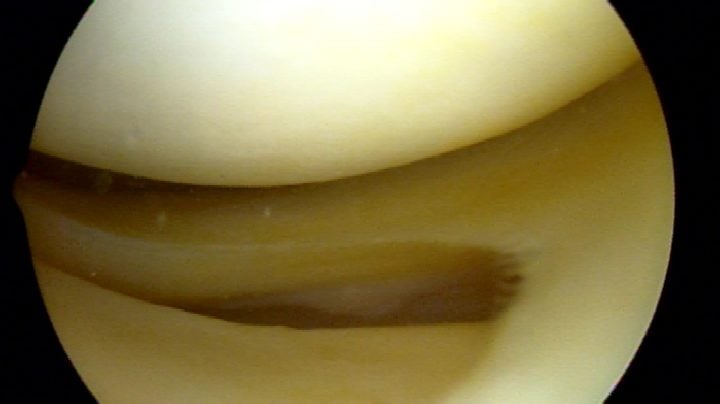
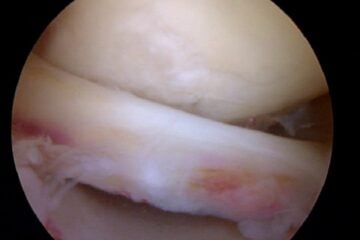
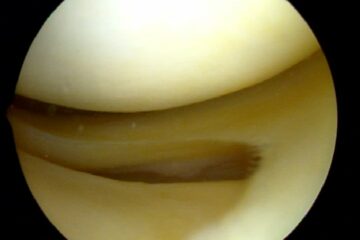
Degenerative tears occur because as we age, or because of our genetics — our tissues simply wear out over time. A degenerative tear is frayed, worn out tissue that looks like the worn out area on the front of your blue jeans. It has very little character, and the tissue is thin, soft, flexible, and looks worn out when we view it at the time of surgery. Most of these changes we see in the meniscus we consider to be “age-appropriate.” We accept thinning hair, the need for glasses, slower running times, and so on… but none of us expect that our internal structures are showing signs of aging too.
For many many years, I have spoken to people about the fact that many meniscus tears, especially degenerative meniscus tears do not often require surgery.
Do I Need Surgery For a Degenerative Meniscus Tear?
Many patients are under the assumption that because something is torn, therefore it must be fixed. That is not the case for many issues in Orthopedic Surgery. This paper on the non-surgical management of degenerative meniscus tears versus surgical management is yet another in a series of papers that supports the non-surgical management of degenerative meniscus tears, especially in the setting of osteoarthritis. Despite how severe your pain is at the onset of your symptoms, typically within a few weeks, your knee feels much better if managed by physical therapy, ice, heat, and anti-inflammatory medication (if you tolerate it).
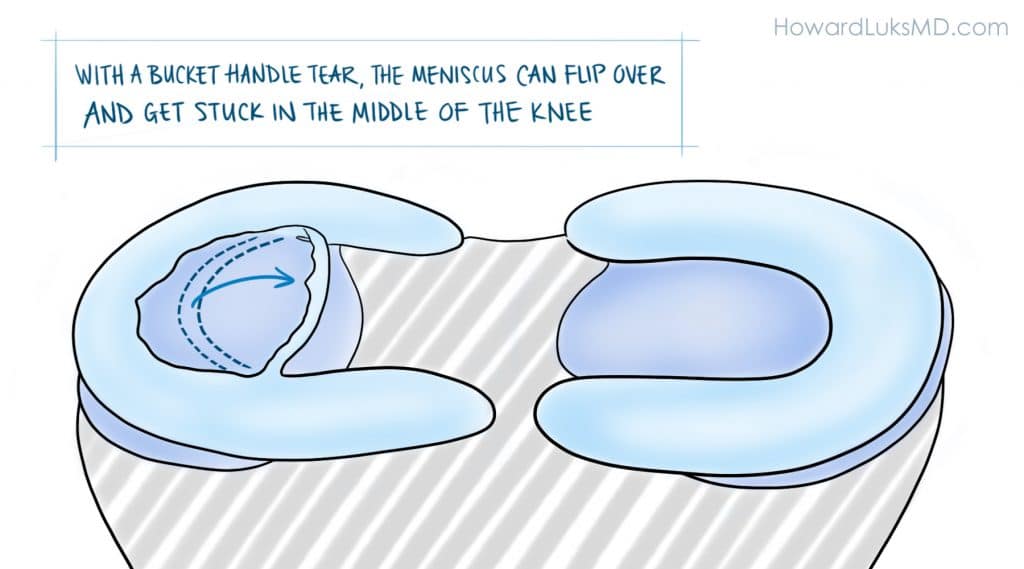
It must be pointed out. The authors of the paper studied degenerative meniscus tears. They did not study the more unusual “radial”, “flap”, or “bucket-handle” tears that can occur in the meniscus. These other tears can be far more “unstable” and produce mechanical symptoms such as instability, buckling, and giving way. In those instances, a meniscal repair, or removal of the torn flap will more than likely be necessary.
This was an important article about the management of this type of meniscus tear, but more studies are necessary. The take-home message is simply that all meniscus tears do not need surgery. Degenerative meniscus tears are usually managed well without surgery.
Have realistic goals about your recovery.
Very few of your orthopedic issues will resolve in less than 3 months. Many of you were told that if your pain persists for 4-6 weeks you should consider surgery. I would suggest that you wait longer than that. With 25 years of treating people under my belt, I can tell you that the majority of people were glad that they waited longer before moving forward with surgery. Surgery might actually bring you closer to a knee replacement. Surgery for degenerative tears will not decrease your chances of developing osteoarthritis. If you do choose to proceed with surgery for a degenerative meniscus tear it should be because:
- your pain persists after a lengthy period of non-surgical management,
- it was a quality of life decision…
- and your surgeon told you that you have little or no arthritis in your knee.
When your visit with your doctor be sure to ask what type of tear you have. If you possess a degenerative tear, without any of the “mechanical” symptoms we mentioned — you should pursue non-surgical treatment at first— and a few months later I think you’ll find that you’re glad that you did.










Hi Dr Luks,
I am a 20 year old female and have been having right knee problems for around a year now. I am in a lot of pain and whenever I extend my knee it cracks. Also it pops when I exercise and sometimes even when I walk. I just got an MRI that said “Tiny 2 mm focus of linear signal contacting the femoral surface of the posterior horn of the medial meniscus, possibly a tiny nondisplaced tear. Please correlate with any medial joint line symptomatology. No large or dominant tear.” What does this mean? Do I need surgery?
Thanks
very unlikely
Hi Dr Luks,
I second the person before me and thank you for taking the time for making a very informative website and answering questions! I am a physical therapist, competitive runner, just turned 30, and really will do anything to keep the longevity of my knee! I have seen a few Dr’s in the past for recurrent pain to my R knee, however I have had conflicting reports at times. A brief history: recurrent bouts of medial hamstring tendinitis and pes anserine bursitis. Then, 2012 while running sprints on woodchip trails landed and felt pop in the posterior medial aspect my knee. It felt like my hamstring tendon, had s&s of hamstring pathology minus any bruising. Had a unremarkable MRI 1 month later, but did notice a possible bakers cyst in that knee. I got back to running, skiing, lifting weights with no problem.
18 months later, 2014 my knee started hurting insidiously again ( I was running a lot on snow however). Symptoms reminded me of pes anserine, but I had joint line tenderness also. I was able to run relatively pain free after a few weeks of rest. Had an MRI (without contrast) acouple months after initial symptoms. Radiology Report stated: abnormal vertical signal in far peripheral red zone and the posterior horn. I suspect a vertical tear of the far posterior horn of the medial meniscus largely extending to the femoral articulate surface. Body of medial meniscus normal. I saw 3 sports medicine ortho dr’s for opinions because one of them said it was a flap tear in the a vascular zone. Could reading of a MRI show that much discrepancy? Flap vs vertical, Avascular vs vascular? I was confused! Needless to say, I took a month off of doing anything that strenuously engaged my hamstrings. it got better, returned full time to athletic activities.
Another 18 months later, or 6 weeks ago, it started hurting gradually over the course of a week. Again reminded me of pes symptoms. I ran a lot of speed intervals the next week and woke up one day withy out 1cm of swelling and primarily patella femoral symptoms. Over 3 days it felt a bit better, so I decided to do the race I had planned. It was a flat out and back course with no turns. I was able to do it, but the next day forth has been bad. I was unable to bend my knee or put much weight in it. Took several weeks until I could bend my knee open chain) with hamstring and joint line pain. 6 weeks and I still have pain with walking, running, medial hamstring activation ( which is very inhibited and has atrophied)….basically the last 15 degrees of extension with eccentric loading of hamstrings replicates my pain ( worse with closed chain, but also feel it in open chain). I have no pain with squatting, going up stairs, and keeping me knee fully flexed actually decreases my pain.
I have to hold off getting an MRI for another month because of a move, so it has been stressing me a lot on what I should or shouldn’t do in the mean time! With my history, and previous MRI, could I have return that “partially healing torn meniscus”, if it ever healed on its own at all. Could the degenerative changes from chronic medial hamstring tendon issues lead to the meniscus tear/ preventing it from healing because I keep activating my hamstrings when I attempt to run/bike/swim. I know some fibers of the hamstring connect into the medial meniscus, this is why I am wondering!
Very long post, sorry! But after seeing a few highly reputable orthos in the past, I’m nervous about what is the right path to take. Surgery, conservative, use of stem cells or prp injections. I have heard a mix of it all. Iwould really appreciate your thoughts on this! Thank you!!
HI ..
I think your follow up MRI is going to be important to see what has happened to the meniscus. Feel free to check back then after an exam and repeat imaging.
Reading the posts and your response I find very helpfuk. I am 46 and went dancing at a wedding.l back in Sept. Line dancing involved alot of turns and by night I was in pain. Tha next day I could not walk. I went and got a MRI sbout 10 days later and it stated I had small moderate joiny effusion, tiny bakers cyst, synovitis, cartilage irregularity involving the patellofemoral compartment and tear posterior horn and midbody medial menuscus. Well the doctor recommended surgery but I read your post that same day. I scheduled surgery for mid november and wanted to give it a total of 8 weeks to see how it feel. Now I am walking better, much better and it has been 4 weeks since the pain started and I have 4 more weeks before surgery. I take ibuprofen every now and then. I have to position my knee a certain way when sleeping but it is getting better. I need to excercise and the weather is changing so i will need to walk real slow on a treadmill. I will see how well I am doing after walking on the treadmill gradually. Thank you souch for your advice because the doctor and people I talked to had me scared.
I think you know the answer to that question… this is more often than not a quality of life decision.
Hi Dr. Luks
I would really appreciate your advice on this. I work in Africa, having surgery (as suggested by the doctors here) in home country would require some planning, and would like to make sure that surgery is an absolute must.
I injured my left knee in May 2014 by twisting it whilst landing (I was playing volleyball). It was very painful at the time. Pain gradually subsided as I used anti-inflammatory medication, a knee holder, ice. I do yoga, pilates regularly and on one or two occasions it was slightly painful when doing exercises that put pressure on the knee. In July this year, the knee got swollen and was painful for about a week. Pain kicked in a few days after carrying a heavy bag down nine floors. Pain subsided with the same treatment as above, and since then I have been able to continue exercising regularly without any issues. Some of the pilates poses would be trying for the knee but I have felt no pain. Just over a week ago, I started feeling pain again after walking for about 30 minutes whilst carrying something heavy on left shoulder. Pain kicked in after a day or two, and gradually got worse. This time it was also more intense than on the second occasion especially at night and was not able to sleep on the side. Pain is subsiding after a week. The MRI results are:
– abnormality of linear signal of the posterior horn of the meniscus in contact with its internal tibial articular surface resulting in a decisive meniscal lesion of grade 3. The crossed ligaments are in place and have a normal morphology. Integrity of the tendons of the crow’s feet. No internal meniscal lesion. No intra-articular effusion. No abnormal bone structures. Conclusion: Grade 3 lesion of the posterior horn of the internal meniscus (this is a translation of the results).
The local GP and orthopedist advise that surgery is necessary asap. Again, your advice would be very much appreciated.
Thank you.
PS. I’m a 39 years old female and would like to continue to be able to exercise.
Meniscus tears like this are certainly not emergencies. If the pain limits you then surgery to repair it (stitch it) is ok to consider. Exercises in one plane or direction are ok and generally well tolerated. Turning, pivoting, twisting, deep squatting might bother you and potentially (small chance) make the tear larger.
Many thanks for the quick reply. This is my dilemma – the pain does not bother me, in general, but it did surface three times within a year. After the initial injury, it seems to be brought on by carrying something heavy. If I avoid this, would I be able to continue doing yoga, pilates without making the tear worse. And what does worse, larger tear mean? what would be the consequences of that. Thank you for your time.