
Recovery from ACL surgery should be considered a marathon and not a sprint. The recovery process actually begins before ACL surgery. After surgery, the first four weeks of your ACL recovery will lay the groundwork for the ensuing 6-8 months.
This is a follow-up article to an original post intended to help educate those who have experienced an anterior cruciate ligament (ACL) injury and are looking to become better educated on the rehab and physical therapy that follows.
The first four weeks really sets the stage for a successful rehab and allow a smoother rehab for the several weeks and months that follow. The following tips are key takeaways as an experienced physical therapist specializing in rehabbing individuals with an ACL injury looking to return to high level sport and a very active lifestyle.
1. Get the pain under control early & beware of GI issues
It is realistic to set a goal with patients to be entirely off of pain medication within 1 week of surgery, but take care to respect the early pain. The first 48-72 hours following surgery must prioritize pain and symptom management. There is far greater success with patients slowly lowering the amount of pain medication gradually than trying to spread the time between doses too far and too early as they try to wean off pain meds. The pain medication “river” should flow stronger at the beginning of the week and then become shallower yet continuous as the week goes on before drying up completely. Those who try to “chase the pain” (only taking meds once symptoms spike) have a difficult time with comfort, muscle guarding, and range of motion later on. Poor pain management early in the rehab process sets the stage for a very negative and fearful perception of pain later making confidence in return to play activities more difficult.
The one piece of advice that is often forgotten or never provided? Make sure you are being very proactive with fiber. Narcotics and constipation often go hand and hand; topping it off with a painful knee will make life miserable. Plan ahead!
2. Get started right away

Pain and symptom management is still the main priority these first three days, but you can get a lot of work in without flaring up symptoms. Muscle facilitation, range of motion, and weight bearing can all occur with clear communication between patient and physical therapist regarding pain levels. I typically tell patients that pain under 3-4/10 is acceptable (can be viewed as good or productive pain) and often times needed, but to refrain from activities or progressions that cause 6/10 pain or higher. Building trust and a more positive perception of pain leads to a very productive first month of rehab. Clear forward progress is a confidence builder for the patient as well and key contributor to rehab compliance.
3. Start viewing your surgical side as an equal.
The positive psychology of ACL rehab is the least talked about, yet the most valuable weapon for physical therapist and patient alike. The quicker a patient starts viewing the surgical side as an equal, not as injured or broken, the smoother the rehab process going forward. This begins with positive self-talk and the PT should model this behavior from the start. Instead of referring to the surgical side as the bad or injured side, simply call it the left or right leg. Eliminate the broken, injured, fragile connotations as soon as possible and watch how pain becomes less of an issue and functionality flourishes. Instead of making the injury the center of the patient’s universe of things they cannot do, let’s put the focus on all the things that can be done while still respecting the healing process. Players on a team do not get better by sitting on the bench, they need opportunities to train – the same goes for the ACL reconstructed knee. Let it participate!
One easy trick to facilitate equal responsibility of limbs is using two bathroom scales, one under each leg and have them find what they think is equal weight bearing. I get patients appreciating what equal weight bearing is as early in the process as possible while also staying respectful of surgical procedures. Providing encouragement to shift weight onto the surgical side while standing despite their first instinct to shift away from that side as a protective mechanism prevents compensatory habits later on complicating walking, squatting, running, jumping, and decelerating.
In addition, I wean patients off post-surgical braces for ambulation as soon as they show adequate quad strength to support their body weight safely on one leg. The brace subconsciously reinforces the habit to not trust the surgical side and also inhibits proper gait mechanics. I will typically keep patients using crutches with full weight bearing longer than their use of a brace so they still have some outside support if they need it, but can begin normalizing their ambulation as soon as possible. Building trust of the surgical side early in the process pays dividends months later.
4. Become a master of full range of motion.
Once pain is managed early, a get-to-work mindset is established, and a positive view of the surgical limb is place, a patient can and should make a significant amount of progress with range of motion without it being an overly painful experience. Range of motion work is a lot like guiding a mule down a path – you need to guide it. If you force it, you will meet resistance (pain, swelling, and ROM loss) and a lot of frustration. If you go into the tightness without trying to go through significant tightness/ pain you will make sustained and consistent progress. Rarely do I have to physically help with a patient’s range of motion; I give the parameters of staying away from 6/10 or higher and encourage 3-4 sessions of extension and flexion ROM work daily through the first several weeks of rehab and motion comes.
Do you have questions regarding an Orthopedic injury or longevity?
Do you want to talk to an expert who can listen to you for 45-60 minutes and explain the options in detail?
Dr. Howard Luks offers remote guidance sessions to review your X-ray or MRI images and explain your options.
Dr. Luks has also received hundreds of requests for educational sessions on the topics discussed in his book, Longevity Simplified.
Those who achieve full and symmetrical active range of motion in extension and flexion within the first 4 weeks typically have less difficulty later on with anterior knee pain, chronic swelling, abnormal gait mechanics, and secondary complications.
Please take note, this is a general opinion for a straight forward ACL reconstruction without additional injury and not intended as specific medical advice. Individuals should always consult with their health care provider about their specific situation and medical care.
Julie Eibensteiner PT, DPT, CSCS is a physical therapist and founder of Laurus Rehab and Performance, an independent physical therapy practice specializing in ACL injuries of competitive athletes in the greater Minneapolis-St. Paul area. www.laurusrehab.com
Twitter: @laurusrehab
Facebook: www.facebook.com/ACLRehab

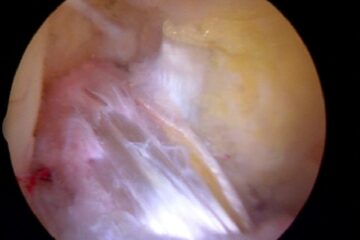
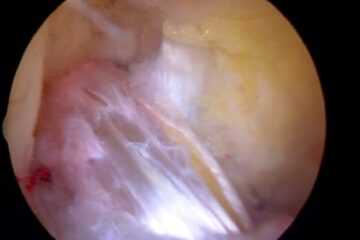






George
I am 16 days post op and I have started walking with one crutch and trying to put full weight on my leg and knee. I can straighten the leg but have limited range of motion at the moment thought better than week 1. The knee pain and swelling is very minimal thus only taking pain meds prior to phsyio appointment. My quad muscle has only begun contracting eith physio electric stimulation. My question is it normal and expected to feel some instability and weakness in the knee when walking ? The knee feeling like it wants to come forward from time to time? If there is something wrong or a re-tear with the graft this early what should I expect to feel and see with my knee.
Thank you for your help,
George
Hi …
Many people do feel that their knee is weak immediately after surgery. That usually continues for a few weeks until your quadriceps starts functioning more effectively. Your doctor can tell you if the new ACL feels loose. That is a physical examination issue.
Rohan Ganguly
I am 3 weeks post op after a acl and meniscus surgery..I’m completely off crutches and can walk around slowly with a small limp…my question is at times while walking I feel a slight twist on the operated knee with slight pain which goes away instantly..Is it normal? I do my PT regularly and walk around as instructed by my surgeon…I plan to join office next week but am worried about the slight twist feeling once in a while.
Sorry Rohan… without examining you I don’t know.
Liza
I’m 8 weeks post op and still have a limp and knee pain. How are you feeling now? How many months are you post op?
Jake White
One of our athletes just experienced an ACL injury, and I wanted to read more about the healing process for an injury of that nature. It sounds like a very careful recovery program, and hopefully he can work on becoming a master of full range motion. I probably won’t anticipate him coming back anytime this season after reading this, so as to give him time to heal. Thanks for sharing!